- About
- Mission Statement
Education. Evidence. Regrowth.
- Education.
Prioritize knowledge. Make better choices.
- Evidence.
Sort good studies from the bad.
- Regrowth.
Get bigger hair gains.
Team MembersPhD's, resarchers, & consumer advocates.
- Rob English
Founder, researcher, & consumer advocate
- Research Team
Our team of PhD’s, researchers, & more
Editorial PolicyDiscover how we conduct our research.
ContactHave questions? Contact us.
Before-Afters- Transformation Photos
Our library of before-after photos.
- — Jenna, 31, U.S.A.
I have attached my before and afters of my progress since joining this group...
- — Tom, 30, U.K.
I’m convinced I’ve recovered to probably the hairline I had 3 years ago. Super stoked…
- — Rabih, 30’s, U.S.A.
My friends actually told me, “Your hairline improved. Your hair looks thicker...
- — RDB, 35, New York, U.S.A.
I also feel my hair has a different texture to it now…
- — Aayush, 20’s, Boston, MA
Firstly thank you for your work in this field. I am immensely grateful that...
- — Ben M., U.S.A
I just wanted to thank you for all your research, for introducing me to this method...
- — Raul, 50, Spain
To be honest I am having fun with all this and I still don’t know how much...
- — Lisa, 52, U.S.
I see a massive amount of regrowth that is all less than about 8 cm long...
Client Testimonials150+ member experiences.
Scroll Down
Popular Treatments- Treatments
Popular treatments. But do they work?
- Finasteride
- Oral
- Topical
- Dutasteride
- Oral
- Topical
- Mesotherapy
- Minoxidil
- Oral
- Topical
- Ketoconazole
- Shampoo
- Topical
- Low-Level Laser Therapy
- Therapy
- Microneedling
- Therapy
- Platelet-Rich Plasma Therapy (PRP)
- Therapy
- Scalp Massages
- Therapy
More
IngredientsTop-selling ingredients, quantified.
- Saw Palmetto
- Redensyl
- Melatonin
- Caffeine
- Biotin
- Rosemary Oil
- Lilac Stem Cells
- Hydrolyzed Wheat Protein
- Sodium Lauryl Sulfate
More
ProductsThe truth about hair loss "best sellers".
- Minoxidil Tablets
Xyon Health
- Finasteride
Strut Health
- Hair Growth Supplements
Happy Head
- REVITA Tablets for Hair Growth Support
DS Laboratories
- FoliGROWTH Ultimate Hair Neutraceutical
Advanced Trichology
- Enhance Hair Density Serum
Fully Vital
- Topical Finasteride and Minoxidil
Xyon Health
- HairOmega Foaming Hair Growth Serum
DrFormulas
- Bio-Cleansing Shampoo
Revivogen MD
more
Key MetricsStandardized rubrics to evaluate all treatments.
- Evidence Quality
Is this treatment well studied?
- Regrowth Potential
How much regrowth can you expect?
- Long-Term Viability
Is this treatment safe & sustainable?
Free Research- Free Resources
Apps, tools, guides, freebies, & more.
- Free CalculatorTopical Finasteride Calculator
- Free Interactive GuideInteractive Guide: What Causes Hair Loss?
- Free ResourceFree Guide: Standardized Scalp Massages
- Free Course7-Day Hair Loss Email Course
- Free DatabaseIngredients Database
- Free Interactive GuideInteractive Guide: Hair Loss Disorders
- Free DatabaseTreatment Guides
- Free Lab TestsProduct Lab Tests: Purity & Potency
- Free Video & Write-upEvidence Quality Masterclass
- Free Interactive GuideDermatology Appointment Guide
More
Articles100+ free articles.
-
10 Best Shampoos for Thinning Hair Men
-
Does Semaglutide Cause Hair Loss?
-
Does Dandruff Cause Hair Loss?
-
Topical Finasteride: The Best Dosage for Maximizing Regrowth and Minimizing Side Effects
-
Ulo Review: #1 Customized Hair Loss Treatment in 2026
-
10 Best Hair Loss Treatments for Men
-
Best Minoxidil for Men: Top Picks for 2026
-
Does Ozempic Cause Hair Loss?
PublicationsOur team’s peer-reviewed studies.
- Microneedling and Its Use in Hair Loss Disorders: A Systematic Review
- Use of Botulinum Toxin for Androgenic Alopecia: A Systematic Review
- Conflicting Reports Regarding the Histopathological Features of Androgenic Alopecia
- Self-Assessments of Standardized Scalp Massages for Androgenic Alopecia: Survey Results
- A Hypothetical Pathogenesis Model For Androgenic Alopecia:Clarifying The Dihydrotestosterone Paradox And Rate-Limiting Recovery Factors
Menu- AboutAbout
- Mission Statement
Education. Evidence. Regrowth.
- Team Members
PhD's, resarchers, & consumer advocates.
- Editorial Policy
Discover how we conduct our research.
- Contact
Have questions? Contact us.
- Before-Afters
Before-Afters- Transformation Photos
Our library of before-after photos.
- Client Testimonials
Read the experiences of members
Before-Afters/ Client Testimonials- Popular Treatments
-
Articles
Explore the science behind hair loss and hair growth. Our in-depth articles cover topics ranging from natural remedies to pharmaceuticals to breakthroughs in hair loss science. Want to request an article topic? Contact us.
IngredientsPharmaceuticalsNatural RemediesCompany Reviews By Sophie Grice, PhDMay 23, 2026
By Sophie Grice, PhDMay 23, 202610 Best Shampoos for Thinning Hair Men
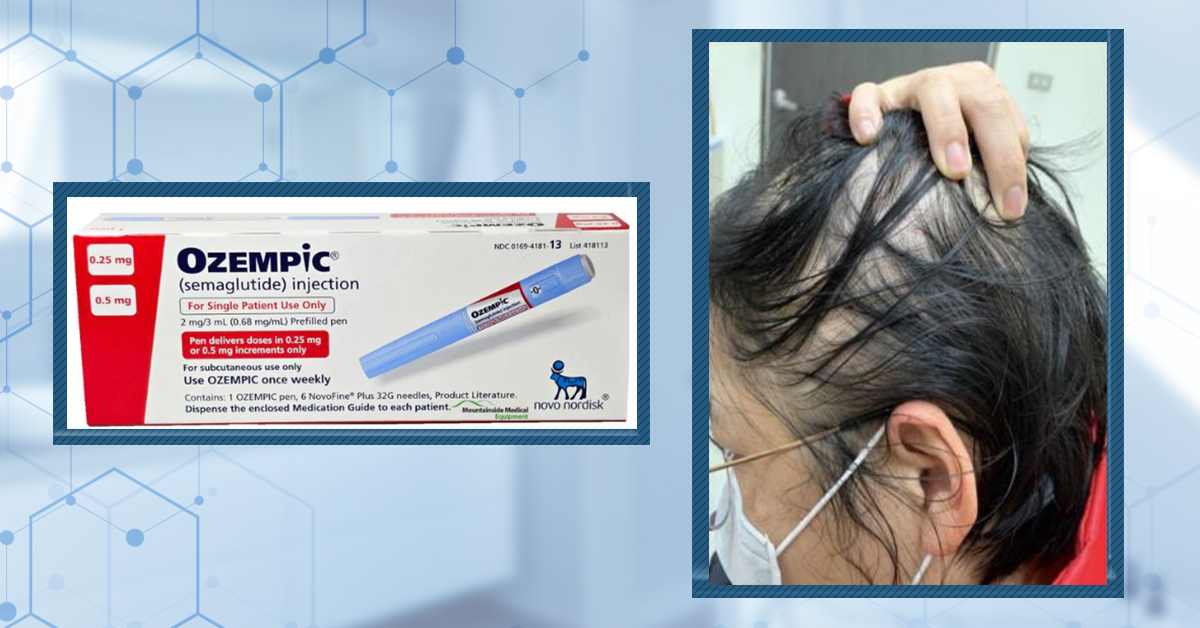
If you’re looking into products for thinning hair, shampoos are often one of the first options to consider. They’re quick, convenient, and easy to add into a routine. But a lot of these products rely on heavy marketing, and only a handful of ingredients actually have clinical evidence behind them in...By Cassie Hopton, PhDMay 22, 2026Does Semaglutide Cause Hair Loss?
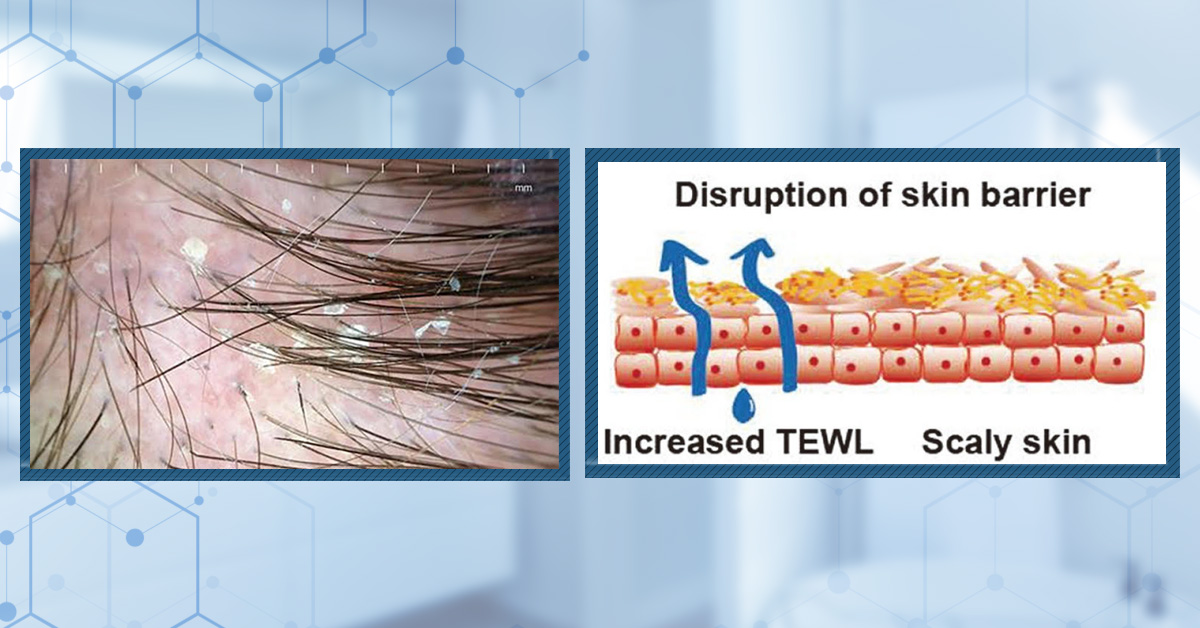
GLP-1 medications like semaglutide have transformed obesity and diabetes treatment, helping millions lose weight and improve metabolic health. But some users report an unexpected side effect: hair shedding. Is semaglutide actually responsible? In this article, we explore the scientific evidence, the...By Cassie Hopton, PhDMay 15, 2026Does Dandruff Cause Hair Loss?
Dandruff is more than a cosmetic nuisance: it often reflects scalp inflammation that can disrupt the hair cycle. While dandruff itself doesn’t directly cause hair loss, it may trigger shedding and worsen conditions like pattern hair loss. Understanding the root cause of dandruff and treating it effe...By Perfect Hair Health TeamMay 15, 2026Topical Finasteride: The Best Dosage for Maximizing Regrowth and Minimizing Side Effects
Since earning FDA approval in 1997, Finasteride has been one of the most widely used hair loss drugs. To avoid potential sexual side effects, many opt for topical finasteride in hopes of isolating the drug’s DHT-reducing effects on the scalp. However, at certain doses, topical finasteride can enter ... By Dr. Michael WilliamsMay 9, 2026
By Dr. Michael WilliamsMay 9, 2026Ulo Review: #1 Customized Hair Loss Treatment in 2026
Ulo, co-founded by Perfect Hair Health, was created to address long-standing issues in the hair loss industry, from unsafe formulations to misleading personalization claims. In this review, we examine whether Ulo’s evidence-first, highly customizable approach truly sets a new benchmark for hair loss...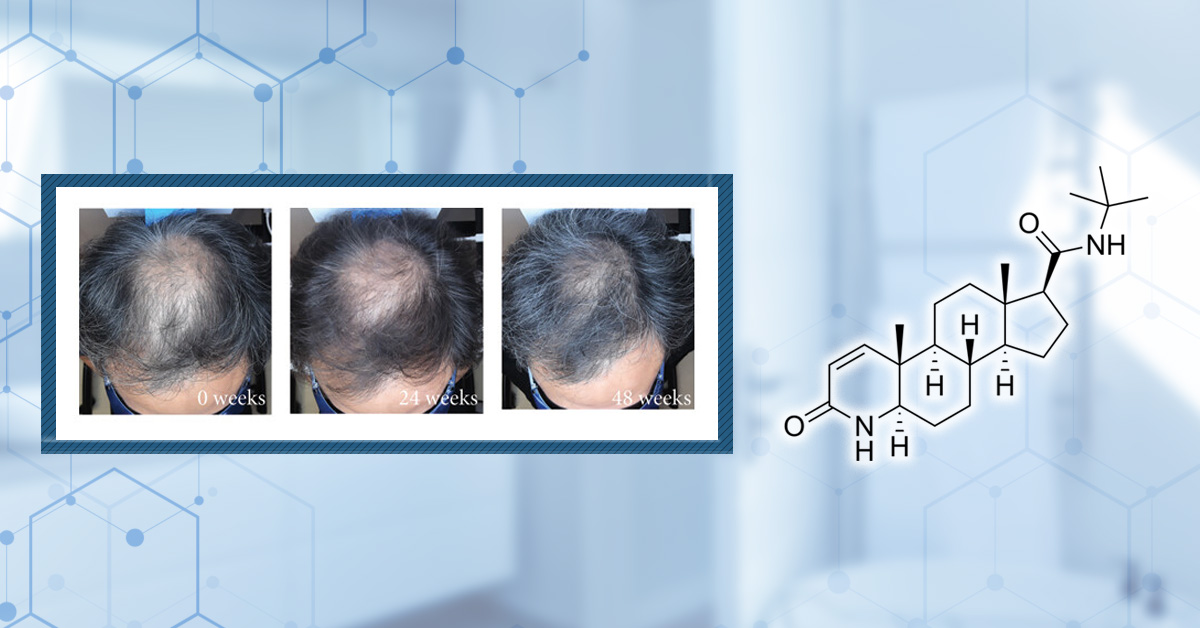 By Sophie Grice, PhDMay 8, 2026
By Sophie Grice, PhDMay 8, 202610 Best Hair Loss Treatments for Men
If you are at the start of your hair-loss journey, figuring out where to begin can feel overwhelming. There is no shortage of products and treatments that promise results, but not all of them are worth your time and money. In this article, we break down 10 of the best hair loss treatments for men, i... By Sarah King, PhDMay 7, 2026
By Sarah King, PhDMay 7, 2026Best Minoxidil for Men: Top Picks for 2026
With countless hair loss products on the market, choosing the right minoxidil can be overwhelming. This evidence-based guide ranks the best minoxidil treatments for men in 2026, including prescription and over-the-counter options, based on effectiveness, safety, customization, and value. Discover wh...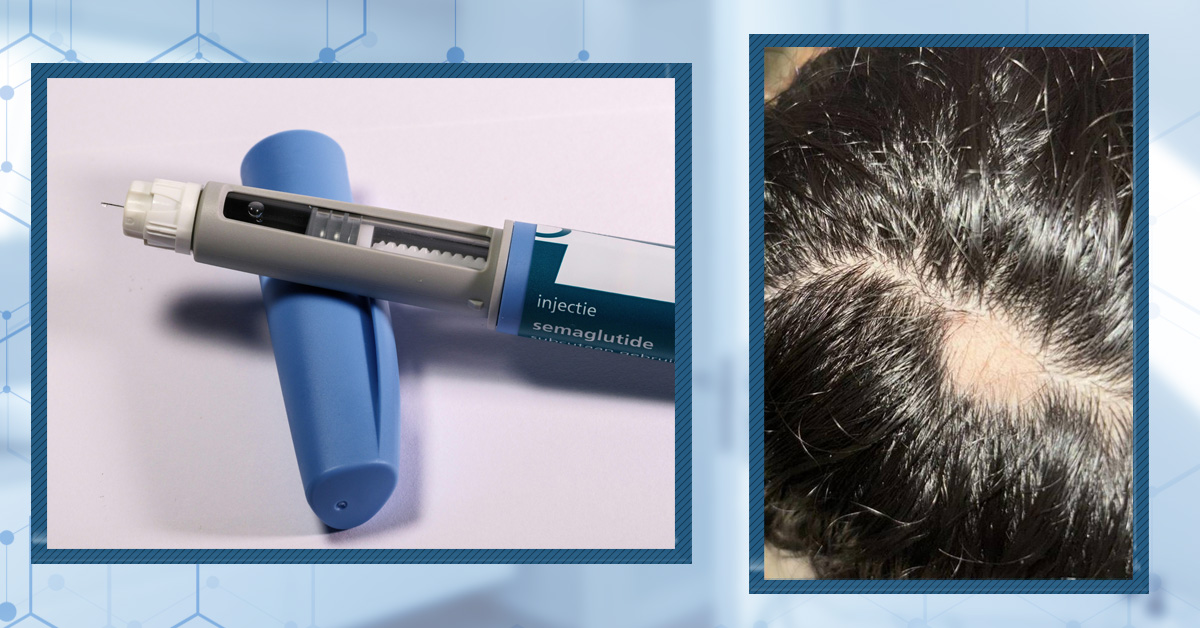 By Catherine Kennedy, PhDMay 1, 2026
By Catherine Kennedy, PhDMay 1, 2026Does Ozempic Cause Hair Loss?
GLP-1 medications like Ozempic are transforming weight-loss treatment. But viral posts and patient reports have raised concerns about unexpected hair shedding, and emerging research hints there may be something to it. But what does the science really show? We unpack the latest evidence to examine wh...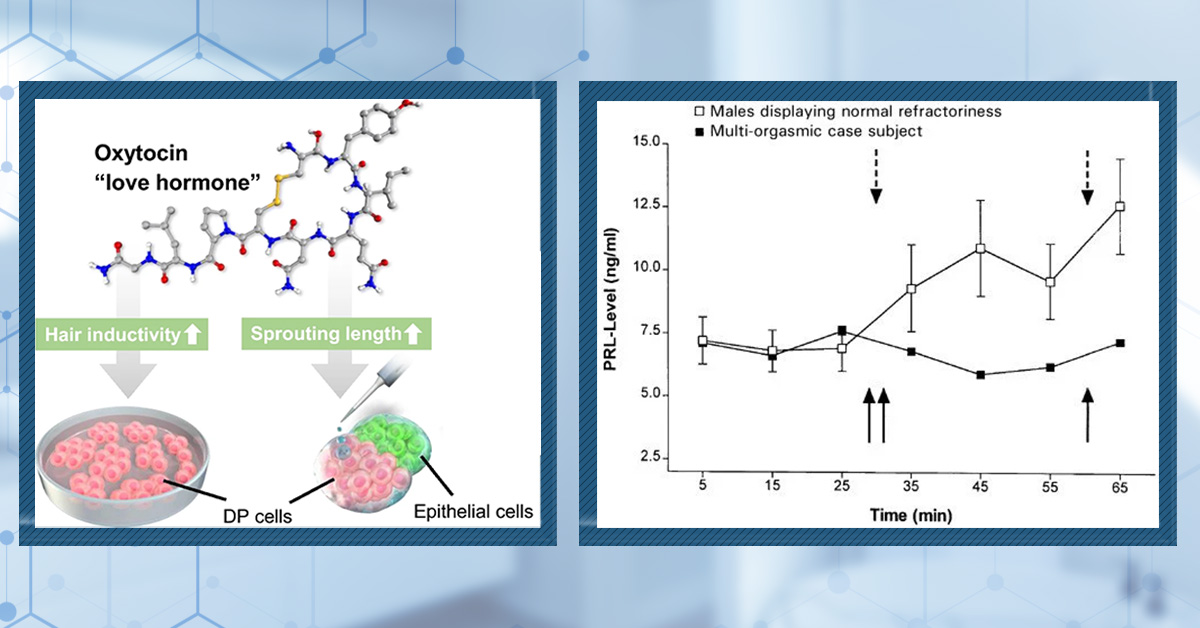 By Dr. Michael WilliamsApr 30, 2026
By Dr. Michael WilliamsApr 30, 2026Does Masturbation Cause Hair Loss?
Theories about the causes of hair loss abound online. A potential link with masturbation is among the more curious of these ideas. Interestingly, there is a range of molecular mechanisms that may form the biological basis for the connection between masturbation and hair loss. But do they stand up to... By Cassie Hopton, PhDApr 24, 2026
By Cassie Hopton, PhDApr 24, 20266 Best Hair Loss Treatments for Women
Female pattern hair loss treatments vary widely in effectiveness, safety, and suitability across life stages. In this evidence-based guide, we review six of the best options for women, from minoxidil to low-level laser therapy, explaining how they work, the clinical evidence behind them, key safety ...Stop guessing which hair loss
treatments actually workInstead, just read our cheat sheet
You’ll get the facts on nine “natural” and “conventional” hair loss treatments: how they work, how much hair they’ll regrow, their limitations, and what their marketers don’t want you know.
- Mission Statement
 Scroll Down
Scroll Down