- About
- Mission Statement
Education. Evidence. Regrowth.
- Education.
Prioritize knowledge. Make better choices.
- Evidence.
Sort good studies from the bad.
- Regrowth.
Get bigger hair gains.
Team MembersPhD's, resarchers, & consumer advocates.
- Rob English
Founder, researcher, & consumer advocate
- Research Team
Our team of PhD’s, researchers, & more
Editorial PolicyDiscover how we conduct our research.
ContactHave questions? Contact us.
Before-Afters- Transformation Photos
Our library of before-after photos.
- — Jenna, 31, U.S.A.
I have attached my before and afters of my progress since joining this group...
- — Tom, 30, U.K.
I’m convinced I’ve recovered to probably the hairline I had 3 years ago. Super stoked…
- — Rabih, 30’s, U.S.A.
My friends actually told me, “Your hairline improved. Your hair looks thicker...
- — RDB, 35, New York, U.S.A.
I also feel my hair has a different texture to it now…
- — Aayush, 20’s, Boston, MA
Firstly thank you for your work in this field. I am immensely grateful that...
- — Ben M., U.S.A
I just wanted to thank you for all your research, for introducing me to this method...
- — Raul, 50, Spain
To be honest I am having fun with all this and I still don’t know how much...
- — Lisa, 52, U.S.
I see a massive amount of regrowth that is all less than about 8 cm long...
Client Testimonials150+ member experiences.
Scroll Down
Popular Treatments- Treatments
Popular treatments. But do they work?
- Finasteride
- Oral
- Topical
- Dutasteride
- Oral
- Topical
- Mesotherapy
- Minoxidil
- Oral
- Topical
- Ketoconazole
- Shampoo
- Topical
- Low-Level Laser Therapy
- Therapy
- Microneedling
- Therapy
- Platelet-Rich Plasma Therapy (PRP)
- Therapy
- Scalp Massages
- Therapy
More
IngredientsTop-selling ingredients, quantified.
- Saw Palmetto
- Redensyl
- Melatonin
- Caffeine
- Biotin
- Rosemary Oil
- Lilac Stem Cells
- Hydrolyzed Wheat Protein
- Sodium Lauryl Sulfate
More
ProductsThe truth about hair loss "best sellers".
- Minoxidil Tablets
Xyon Health
- Finasteride
Strut Health
- Hair Growth Supplements
Happy Head
- REVITA Tablets for Hair Growth Support
DS Laboratories
- FoliGROWTH Ultimate Hair Neutraceutical
Advanced Trichology
- Enhance Hair Density Serum
Fully Vital
- Topical Finasteride and Minoxidil
Xyon Health
- HairOmega Foaming Hair Growth Serum
DrFormulas
- Bio-Cleansing Shampoo
Revivogen MD
more
Key MetricsStandardized rubrics to evaluate all treatments.
- Evidence Quality
Is this treatment well studied?
- Regrowth Potential
How much regrowth can you expect?
- Long-Term Viability
Is this treatment safe & sustainable?
Free Research- Free Resources
Apps, tools, guides, freebies, & more.
- Free CalculatorTopical Finasteride Calculator
- Free Interactive GuideInteractive Guide: What Causes Hair Loss?
- Free ResourceFree Guide: Standardized Scalp Massages
- Free Course7-Day Hair Loss Email Course
- Free DatabaseIngredients Database
- Free Interactive GuideInteractive Guide: Hair Loss Disorders
- Free DatabaseTreatment Guides
- Free Lab TestsProduct Lab Tests: Purity & Potency
- Free Video & Write-upEvidence Quality Masterclass
- Free Interactive GuideDermatology Appointment Guide
More
Articles100+ free articles.
-
Does Dandruff Cause Hair Loss?
-
Topical Finasteride: The Best Dosage for Maximizing Regrowth and Minimizing Side Effects
-
Ulo Review: #1 Customized Hair Loss Treatment in 2026
-
10 Best Hair Loss Treatments for Men
-
Best Minoxidil for Men: Top Picks for 2026
-
Does Ozempic Cause Hair Loss?
-
Does Masturbation Cause Hair Loss?
-
6 Best Hair Loss Treatments for Women
PublicationsOur team’s peer-reviewed studies.
- Microneedling and Its Use in Hair Loss Disorders: A Systematic Review
- Use of Botulinum Toxin for Androgenic Alopecia: A Systematic Review
- Conflicting Reports Regarding the Histopathological Features of Androgenic Alopecia
- Self-Assessments of Standardized Scalp Massages for Androgenic Alopecia: Survey Results
- A Hypothetical Pathogenesis Model For Androgenic Alopecia:Clarifying The Dihydrotestosterone Paradox And Rate-Limiting Recovery Factors
Menu- AboutAbout
- Mission Statement
Education. Evidence. Regrowth.
- Team Members
PhD's, resarchers, & consumer advocates.
- Editorial Policy
Discover how we conduct our research.
- Contact
Have questions? Contact us.
- Before-Afters
Before-Afters- Transformation Photos
Our library of before-after photos.
- Client Testimonials
Read the experiences of members
Before-Afters/ Client Testimonials- Popular Treatments
-
ArticlesVitamin E For Hair Loss: Fact Versus Fiction (Tocopherols & Tocotrienols)
First Published Jul 23 2020Last Updated Sep 19 2025IngredientsNatural Remedies Researched & Written By:Perfect Hair Health Team
Researched & Written By:Perfect Hair Health Team Reviewed By:Rob English, Medical Editor
Reviewed By:Rob English, Medical Editor
Want help with your hair regrowth journey?
Get personalized support, product recommendations, video calls, and more from our researchers, trichologists, and PhD's dedicated to getting you the best possible outcomes.
Learn MoreArticle Summary
Vitamin E is an essential nutrient and antioxidant, but its usefulness to treat hair loss is incredibly limited. Studies show that vitamin E supplements can improve hair loss caused by nutrient deficiencies, and that topical vitamin E might increase local antioxidant activity in the scalps of people with androgenic alopecia. But there’s also evidence that long-term use of vitamin E is associated with stroke and cancer. Given that fewer than 1% of Americans are deficient in vitamin E, we recommend that you exercise caution before supplementing for hair health.
Full Article
Vitamin E is a cornerstone ingredient in many cosmetic products – especially those marketed to people with hair loss. The rationale from marketers of supplements and topicals? That vitamin E acts as an antioxidant, protects our hair from free radicals, and is clinically studied to improve hair loss outcomes.
So, is there any truth to these claims? Maybe, maybe not.
What’s the relationship between vitamin E and hair health? Can vitamin E promote hair growth? Is it helpful in supplemental and topical form? And are there any risks to supplementation (i.e., cancer) that consumers should know about?
The answers might surprise you… which is why we’ve put together this article.
It’s time to set the record straight on the vitamin E and hair health – so that you can stop getting sucked into marketing gimmicks and start learning the science supporting (or not supporting) the products you’re buying.
All-Natural Hair Supplement
The top natural ingredients for hair growth, all in one supplement.
Take the next step in your hair growth journey with a world-class natural supplement. Ingredients, doses, & concentrations built by science.

What is vitamin E?
Vitamin E is not a single compound. Rather, vitamin E is a family of fat-soluble vitamins (much like the B vitamin family). And this family is best known for its antioxidant activity in fatty tissues and fat-transporting proteins of the body.
The vitamin E family can be segmented into two specific types of vitamin E: tocotrienols and tocopherols.
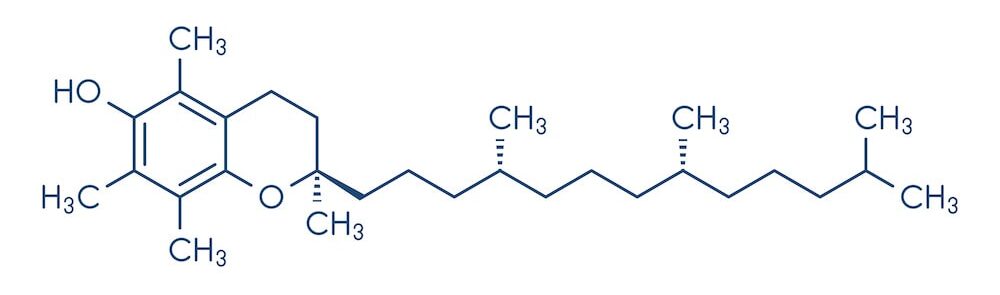
Vitamin E as alpha-tocopheral
Within tocotrienols and tocopherols, there are different vitamin E compounds known as homologues – all of which have varying antioxidant capabilities and roles in the human body.
Perhaps one of the most important roles? These vitamin E homologues help to reduce the activity of reactive oxygen species (ROS). Reactive oxygen species (ROS) are “free radicals” – substances that create inflammation and lead to cellular damage. If ROS activity is elevated for prolonged periods, the damage can eventually impair the function of body tissues.
This can have implications on a variety of organs – including some of our tiniest organs: hair follicles. And this is where a possible connection between vitamin E and hair health begins.
Vitamin E, reactive oxygen species, and hair loss
When reactive oxygen species are elevated, it can create what’s known as oxidative stress (i.e., inflammation). And interestingly, oxidative is implicated in hair loss, and in many ways:
- Oxidative stress can trigger hair shedding
- Oxidative stress is elevated in the scalps of men and women with pattern hair loss
- Oxidative stress is higher in those dealing with stress-related hair loss, like telogen effluvium
Moreover, there are studies suggesting that if we can reduce oxidative stress surrounding our hair follicles, we can also reduce hair shedding, slow down hair follicle miniaturization, and even see some hair regrowth.
This begs the question: is there any evidence that vitamin E can help fight hair loss? After all, vitamin E acts like an antioxidant. Therefore, it’s not unreasonable to believe that vitamin E might help with hair growth.
The rest of this article dives into the evidence.
First, we’ll reveal the studies that marketers reference to sell us vitamin E-containing supplements and topicals. Then, we’ll dissect those studies, tear them to the ground, and discuss why you should think twice about using vitamin E as a hair growth aid.
Vitamin E, hair loss, and hair growth: the evidence in humans
Study (2010): Effects of Tocotrienol Supplementation on Hair Growth in Human Volunteers
In 2010, an investigation team wanted to determine if vitamin E supplements – specifically, tocotrienols and alpha-tocopherols – would help regrow hair for men and women dealing with general hair loss. So, they set up the following study:
- Participants: 38 volunteers (men and women) with hair loss present for at least two months, ranging from “patchy” hair loss to more severe generalized thinning.
- Design: 21 volunteers were given vitamin E pills (100 mg daily); 17 volunteers were given a placebo pill (100 mg daily).
- Measurements: before-after measurements of hair counts and hair weight
After 8 months of supplementing, the investigators assessed the hair growth parameters for both the vitamin E group and the placebo group. The results were impressive.
The vitamin E group saw a 34.5% increase in hair count. And the placebo group? A 0.1% decrease in hair count.
To contextualize just how impressive these results are, finasteride (the gold-standard treatment for male pattern hair loss) increases hair counts by ~10% over a two-year period. So, a 34.5% increase in hair count over eight months is – to put it crudely – 3x the results in less than half the time.
So, does that mean that every hair loss sufferer should start supplementing with vitamin E?
Not necessarily. In fact, there are a few issues with this study that make its results much less impressive than it may seem.
Problem: the investigators don’t tell us the type of hair loss in the study
There are many type of hair loss, and each type corresponds to a different prognosis, a different set of causes, and a different set of treatments.
For instance, nutrient deficiency-related hair loss is temporary and reversible. It occurs predominantly in developing countries, it’s caused by a lack of certain nutrients in the diet, and it’s often reversible through nutrient supplementation.
Male and female pattern hair loss, on the other hand, is chronic and progressive. It occurs mainly in adults, and it’s caused by a combination between genetics, androgens, and a changing scalp environment. Without treatment, it usually gets worse.
Why are these distinctions important? Because they dictate the course of proper treatment. In other words, we can’t apply treatments for nutrient deficiency-related hair loss to people with pattern hair loss… and expect their hair to grow back.
Now, back to that vitamin E study. Who were the volunteers inside that study? And which type of hair loss did they have?
We don’t know.
All we have is a vague description of the volunteers: men and women ages 18-60, living in Malaysia, with varying severities of hair loss ranging from patchy-related hair loss to severe hair thinning.
And herein lies the problem with this vitamin E study:
- Malaysia (where this study was conducted) has an elevated incidence of nutrient deficiencies in its children and adults.
- Many of the Malaysian study volunteers had patchy-related hair loss. This presentation of hair loss is more so related to autoimmunity and nutrient deficiencies, and less so related to pattern hair loss.
- In the developed world, pattern hair loss is the prevailing type of hair loss… and nutrient deficiency-related hair loss occurs much less frequently.
In other words, vitamin E supplementation is probably great for people whose hair loss is caused by a vitamin E deficiency. This is likely much more common in Malaysia than it is the U.S., U.K., Australia, or New Zealand. So, we can’t apply the results of this study to people in other countries – as these people are likely facing a different type of hair loss, which requires a different set of treatments.
Ironically, marketers use this study on vitamin E to sell supplements and topicals to hair loss sufferers in the developed world!
That’s akin to telling someone diet and exercise can reverse all types of diabetes. Yes, this might be true for type II diabetes (which is caused by metabolic syndrome). But it is absolutely not true for type I diabetes (which is caused by genetics / autoimmunity).
Unfortunately, most consumers dealing with hair loss don’t know this. So, they end up buying products containing vitamin E – all without realizing that they might be applying the wrong set of treatments to the wrong type of hair loss.
So, when it comes to treating hair loss, is vitamin E useless?
Not at all!
Remember: vitamin E has been shown to clinically improve hair counts in Malaysian volunteers with hair loss. It’s just that we can’t apply these results to all hair loss sufferers worldwide… mainly because of the unique circumstances – and thereby the unique types of hair loss – faced in Malaysia versus other pockets of the world.
In any case, we can still mechanistically link vitamin E to other types of hair loss. It’s just that we need to balance this with the clinical evidence: how vitamin E might work for hair loss sufferers versus how it actually works. We’ll cover this exercise below.
Vitamin E & hair loss: hypotheses versus realities
To reiterate from earlier, vitamin E acts as an antioxidant; it helps fight free radicals (ROS). And interestingly, free radicals have been implicated in a variety of different hair loss disorders:
- Alopecia areata, a form of autoimmune hair loss characterized by “patchy” hair loss or, in more severe states, loss of eyelashes, eyebrows, and even all body hair
- Pattern hair loss (androgenic alopecia), a patterned form of hair loss characterized by the progressive miniaturization of hair follicles
Given vitamin E is a powerful antioxidant, could it be that vitamin E has the potential to reduce oxidative stress and, in doing so, improve our hair health?
This is what marketers want us to believe. So, they build mechanistic (or hypothetical) arguments to explain why vitamin E supplementation makes sense. In this next section, we’ll build up these arguments and then evaluate them when they’re put to the test (i.e., clinical trials).
Alopecia areata
Could vitamin E help? (Hypothesis)
Studies measuring the blood of alopecia areata patients have consistently found increased oxidative stress (i.e., the overall damage done by free radicals) when compared to healthy control subjects. In other words, alopecia areata patients are more likely to exhibit higher degrees of oxidative stress, or inflammation.
Oxidative stress has recently been linked to the development of autoimmune disorders, including in autoimmunity specific to the skin. This suggests oxidative stress could play a role in initiating autoimmunity in the hair follicles – like alopecia areata. Therefore, antioxidants might help to lower this oxidative stress and thereby treat autoimmune-driven hair loss.
This all implies that vitamin E – which acts like an antioxidant – might be useful in the fight against alopecia areata.
…But does vitamin E help? (Clinical evidence)
We could not find any clinical studies showing that vitamin E (as a supplement or topical) improved hair loss in people with alopecia areata.
While one study found that alopecia areata patients had lower levels of vitamin E when compared to controls, another study found no statistically significant difference between patients and controls. Moreover, in these studies, patients with alopecia areata were not deficient in vitamin E… suggesting that vitamin E supplementation likely wouldn’t have been that useful.
Additionally, it’s not totally clear if reducing oxidative stress is effective at reducing autoimmune forms of hair loss. For instance, evidence suggests that oxidative stress might not be a cause of autoimmunity, but rather a consequence.
As such, it appears that vitamin E supplementation is probably of no benefit to these patients (in fact, there may even be a risk… more on this later).
Pattern hair loss (androgenic alopecia)
Could vitamin E help? (Hypothesis)
Studies investigating the role of oxidative stress in androgenic alopecia (AGA) are sparse. Nonetheless, some studies have posited a potential link:
- One study examined the total oxidant status (TOS), total antioxidant status (TAO), and oxidative stress index (OSI), all measurements of systemic oxidative stress, in young men with AGA. The authors found no difference in TAO, but found significantly higher levels of TOS and OSI, suggesting men with AGA have higher levels of oxidative stress.
- Another study looked at dermal papilla cells (DPCs; the cells that are responsible for maintaining hair growth) from AGA-affected follicles and non-AGA-affected follicles. When exposed to oxidative elements, DPCs from AGA-affected follicles were significantly more susceptible to damage (which could translate to stunted growth) than DPCs from non-AGA-follicles. This suggests susceptibility to oxidative stress may play a role in AGA.
- An additional study examined the role of oxidative stress in the scalps of men with AGA vs their own non-AGA-affected follicles. The findings demonstrate a 2-fold increase in oxidative stress, specifically, among the sebaceous glands of AGA-affected follicles versus the non-AGA-affected follicles. The authors also note that these findings support the hypothesis that oxidative stress may be involved in the growth of sebaceous glands seen in AGA (which means increased oil output… more on the relevance of this in a second).
- Yet another study found that androgen-stimulated transforming growth factor beta-1 (TGF-B1), a protein involved in AGA follicle miniaturization, was dependent on ROS for its activation. By blocking the ROS with an antioxidant, they were also able to block TGF-B1 activation. This suggests that reducing ROS levels may also block follicle miniaturization.
Altogether, the evidence points to a compelling role for oxidative stress in AGA. But, could it be from a vitamin E deficiency?
Probably not.
…But does vitamin E help? (Clinical evidence)
According to the CDC, less than 1% of American adults are vitamin E deficient. So, for the overwhelming majority of AGA patients, vitamin E deficiency isn’t an issue that needs to be addressed.
At the same time, blood work isn’t always a fair measurement of vitamin sufficiencies. For reference, there have been cases of people who had normal blood levels of zinc, but localized zinc deficiencies in the skin. Therefore, these people saw great hair regrowth from zinc supplementation – because they were addressing a zinc deficiency that wasn’t showing up in bloodwork.
So, could the same relationship exist with vitamin E? Maybe. And this is where vitamin E might be useful to AGA patients – more so as a topical than as a supplement.
Androgenic alopecia & localized vitamin E deficiencies: a possible link?
Pattern hair loss, or androgenic alopecia (AGA), is a multi-factorial condition. Yes, genetics and androgens are certainly involved. But there are also additional factors that can contribute to the condition – like our scalp’s environment.
Specifically, researchers have implicated the over-colonization of our scalp’s microflora (microorganisms) as a potential trigger for AGA-related hair shedding. Specifically, these microorganisms can induce significant amounts of oxidative stress in the hair follicle. This oxidative stress can cause hair shedding, and thereby the progression of pattern hair loss.
So, what does this have to do with vitamin E?
Well, some of the most common microorganism overgrowths in AGA-affected scalps are Malassezia spp. (a species of yeast) and Propionibacterium acnes (also known as P. acnes – a pathogenic bacteria).
Interestingly, P. acnes isn’t just implicated in pattern hair loss; it’s also implicated in acne. In fact, studies on acne patients show that they can have depleted levels of vitamin E in their sebum… but normal vitamin E levels in the blood.
In other words, acne patients can have a localized vitamin E deficiency, even if their blood tests show normal vitamin E levels. And this deficiency is a direct result of oxidative stress caused by microorganisms living in the scalp skin.
So, can vitamin E supplementation help increase the vitamin E content in local tissues – like the scalp?
It’s possible.
One study found that over 2-3 weeks, participants taking 400mg daily increased vitamin E sebum levels by 87-92%. We could hypothetically extrapolate this to the scalp skin and suggest that vitamin E might help reduce inflammation caused by local microorganisms in AGA.
At the same time, there are problems with making a recommendation like this. Only 30-70% of AGA sufferers actually have microorganism overgrowths. So, while microorganism overgrowths are definitely partial contributors to AGA-related inflammation, they probably aren’t the primary cause. This means that targeting these overgrowths won’t be useful to everyone.
Secondly (and perhaps more importantly), vitamin E can become toxic if the dose is too high. And, even in normal dosages, its long-term use may increase the risk of certain cancers. That means we should exercise caution before supplementing.
More on that second point below.
Vitamin E supplementation risks: stroke, bleeding disorders, and cancer
Again, most AGA patients don’t have a vitamin E deficiency in the blood. It’s possible that some AGA patients have a local deficiency in balding tissues. At the same time, this is less so related to vitamin E consumption… and more so related to the inflammation from pathogenic bacteria living the scalp skin (which depletes vitamin E). That means that these people should target to kill off these microorganisms (the cause of the deficiency) rather than target to increase vitamin E.
Moreover, when it comes to supplementing with vitamin E without having a deficiency, we also run the risk of vitamin E excess (also known as hypervitaminosis E).
Generally, doses under 1,000mg per day are considered safe. However, this is likely dependent on your baseline vitamin E level (higher starting vitamin E level = less of a dose required to push you over a healthy vitamin E level).
But, in the event that you tip yourself over the threshold (i.e., over 19.9 mg/L daily), there are some serious risks involved:
- A risk of intracranial hemorrhagic stroke. There are at least 3 case reports of this condition caused by vitamin E excess. The serum levels of vitamin E measured in each case were as follows: 23.3 mg/L, 30.8 mg/L, and 46.7 mg/L.
- An increased risk of other bleeding disorders. An imbalance in the vitamin E to vitamin K ratio can interfere with the body’s ability to effectively form blood clots. When vitamin E is too low, it might increase the risk of problematic blood clots. When too high, it may make the blood too thin, leading to bleeding disorders.
- Potentially the opposite of what we’re trying to achieve with vitamin E: oxidative stress. Vitamin E’s antioxidant effects are biphasic and interrelated with other vitamins. When vitamin E increases but vitamin C and CoQ10 don’t, it creates the environment for vitamin E to become pro-oxidant instead of antioxidant. Moreover, high doses of vitamin E may also have a pro-oxidant effect. One study of asthma patients taking 745 IU of vitamin E daily found that vitamin E paradoxically increased oxidative stress.
- Increased risk of cancer. While the relative risk increase was small, one multi-year study on thousands of subjects found that vitamin E supplementation actually increased the risk of high-grade prostate cancer.
- New popular diets depleting polyunsaturated fatty acids (PUFAs) in conjunction with supra-physiological doses of vitamin E may increase these risks. In order to keep PUFAs functioning in the cell (performing immunoregulatory functions and stimulating hair growth, for example), we need vitamin E to prevent them from becoming rancidified in the body. Thus, a higher consumption of PUFAs increases the requirement for vitamin E. But, the converse is also true: a decreased consumption decreases the requirement. For individuals who do choose to lower their PUFA consumption, high doses of vitamin E may increase your risk of vitamin E excess (and the associated risks).
The bottom line: most people aren’t vitamin E deficient, so most people shouldn’t be supplementing. Of the people who have a localized vitamin E deficiency, this isn’t necessarily due to low vitamin E consumption; it’s due to the inflammation generated by pathogenic microorganisms (which deplete vitamin E levels). So, it’s better to target to kill off those bacteria than it is to just supplement with more vitamin E… as doing so can increase the risk of a lot of health detriments.
So, what about the application of topical vitamin E? Could this increase the vitamin E in sebum while circumventing the risks associated with oral supplementation?
Potentially. But again, its usefulness for hair loss sufferers is incredibly narrow.
Human study: 0.1% topical vitamin E increases vitamin E sebum content by almost 300%
In a novel study on human volunteers, the topical application of a cream containing a combination of 0.05% ubiquinone (CoQ10), 0.1% vitamin E, and 1% squalene was applied daily for 2 months.
After the 2 months, the vitamin E measurements in sebum increased by over 280% – almost a 3-fold difference! As such, topical vitamin E application, in concentrations even as low at 0.1%, can directly address the local vitamin E deficiency that’s likely to occur in AGA scalps.
How to mix your own topical vitamin E for hair loss
- Start with a 100% vitamin E oil
- Pick your carrier oil of choice. Coconut oil, black seed oil, pumpkin seed oil, and/or hemp seed oil are all good options.
- In a bottle, preferably a dark, glass bottle with a closure (but plastic works, too), mix the oil and the vitamin E in a 1000:1 to 100:1 ratio (0.1% to 1%). In other words, for a 1% solution, you’ll use 1mL of pure vitamin E for every 100mL of carrier oil. For a 0.1% solution, you’ll use 1mL of pure vitamin E for every 1000mL of carrier oil. This recipe can be adjusted for any size batch you want to do. For smaller batches (say, for 100mL batches at a concentration of 0.1%), you can use a syringe to measure your vitamin E.
- Apply up to 1-2 times daily in areas of hair loss.
- See how things go over the next 3-6 months.
Is topical vitamin E going to help most people achieve hair regrowth?
Probably not.
If you’re dealing with (1) vitamin E deficiency-related hair loss, or (2) androgenic alopecia that coincides with scalp microbial overgrowths (as evidenced by lots of sebum production, dandruff, itching, etc.), then maybe topical vitamin E will help. But again, vitamin E deficiencies are incredibly rare in the developed world. And when it comes to localized vitamin E deficiencies in AGA patients, this is more so the consequence of inflammation from a microbial overgrowth… and less so the cause of hair thinning. So, in addition to a vitamin E topical, you’d also want to kill off that microbial overgrowth (by way of a ketoconazole shampoo or anti-fungal topical.
The verdict on vitamin E
When it comes to fighting hair loss, vitamin E might help:
- People with hair loss from vitamin E deficiencies (in this case, try supplemental vitamin E)
- People with hair loss alongside widespread antioxidant deficiencies (in this case, try supplemental vitamin E)
- People with androgenic alopecia (AGA) who also have secondary scalp inflammation from pathogenic microorganisms (in this case, try 0.1% topical vitamin E).
Vitamin E probably won’t be helpful for:
- People who are not vitamin E deficient
- People who don’t have antioxidant deficiencies
- People with AGA who don’t have microorganism-related secondary scalp inflammation (as evidenced by lots of dandruff and/or sebum)
The bottom line: vitamin E’s usefulness for hair is highly specific. There’s clinical evidence that it might help treat cases of nutrient deficiency-related hair loss and temporary hair loss (i.e., telogen effluvium). There’s hypothetical evidence that it might help replete localized vitamin E deficiencies caused by microorganism overgrowths in AGA. But that’s about it.
Overall, you’re probably better off investing in treatments with better clinical support and better long-term safety profiles.
Have you tried vitamin E for your hair loss? Let us know your experience in the comments below.
Want help with your hair regrowth journey?
Get personalized support, product recommendations, video calls, and more from our researchers, trichologists, and PhD's dedicated to getting you the best possible outcomes.
Learn More
Perfect Hair Health Team
"... Can’t thank @Rob (PHH) and @sanderson17 enough for allowing me to understand a bit what was going on with me and why all these [things were] happening ... "
— RDB, 35, New York, U.S.A."... There is a lot improvement that I am seeing and my scalp feel alive nowadays... Thanks everyone. "
— Aayush, 20’s, Boston, MA"... I can say that my hair volume/thickness is about 30% more than it was when I first started."
— Douglas, 50’s, Montréal, CanadaWant help with your hair regrowth journey?
Get personalized support, product recommendations, video calls, and more from our researchers, trichologists, and PhD's dedicated to getting you the best possible outcomes.
Join Now - Mission Statement
 Scroll Down
Scroll Down