- About
- Mission Statement
Education. Evidence. Regrowth.
- Education.
Prioritize knowledge. Make better choices.
- Evidence.
Sort good studies from the bad.
- Regrowth.
Get bigger hair gains.
Team MembersPhD's, resarchers, & consumer advocates.
- Rob English
Founder, researcher, & consumer advocate
- Research Team
Our team of PhD’s, researchers, & more
Editorial PolicyDiscover how we conduct our research.
ContactHave questions? Contact us.
Before-Afters- Transformation Photos
Our library of before-after photos.
- — Jenna, 31, U.S.A.
I have attached my before and afters of my progress since joining this group...
- — Tom, 30, U.K.
I’m convinced I’ve recovered to probably the hairline I had 3 years ago. Super stoked…
- — Rabih, 30’s, U.S.A.
My friends actually told me, “Your hairline improved. Your hair looks thicker...
- — RDB, 35, New York, U.S.A.
I also feel my hair has a different texture to it now…
- — Aayush, 20’s, Boston, MA
Firstly thank you for your work in this field. I am immensely grateful that...
- — Ben M., U.S.A
I just wanted to thank you for all your research, for introducing me to this method...
- — Raul, 50, Spain
To be honest I am having fun with all this and I still don’t know how much...
- — Lisa, 52, U.S.
I see a massive amount of regrowth that is all less than about 8 cm long...
Client Testimonials150+ member experiences.
Scroll Down
Popular Treatments- Treatments
Popular treatments. But do they work?
- Finasteride
- Oral
- Topical
- Dutasteride
- Oral
- Topical
- Mesotherapy
- Minoxidil
- Oral
- Topical
- Ketoconazole
- Shampoo
- Topical
- Low-Level Laser Therapy
- Therapy
- Microneedling
- Therapy
- Platelet-Rich Plasma Therapy (PRP)
- Therapy
- Scalp Massages
- Therapy
More
IngredientsTop-selling ingredients, quantified.
- Saw Palmetto
- Redensyl
- Melatonin
- Caffeine
- Biotin
- Rosemary Oil
- Lilac Stem Cells
- Hydrolyzed Wheat Protein
- Sodium Lauryl Sulfate
More
ProductsThe truth about hair loss "best sellers".
- Minoxidil Tablets
Xyon Health
- Finasteride
Strut Health
- Hair Growth Supplements
Happy Head
- REVITA Tablets for Hair Growth Support
DS Laboratories
- FoliGROWTH Ultimate Hair Neutraceutical
Advanced Trichology
- Enhance Hair Density Serum
Fully Vital
- Topical Finasteride and Minoxidil
Xyon Health
- HairOmega Foaming Hair Growth Serum
DrFormulas
- Bio-Cleansing Shampoo
Revivogen MD
more
Key MetricsStandardized rubrics to evaluate all treatments.
- Evidence Quality
Is this treatment well studied?
- Regrowth Potential
How much regrowth can you expect?
- Long-Term Viability
Is this treatment safe & sustainable?
Free Research- Free Resources
Apps, tools, guides, freebies, & more.
- Free CalculatorTopical Finasteride Calculator
- Free Interactive GuideInteractive Guide: What Causes Hair Loss?
- Free ResourceFree Guide: Standardized Scalp Massages
- Free Course7-Day Hair Loss Email Course
- Free DatabaseIngredients Database
- Free Interactive GuideInteractive Guide: Hair Loss Disorders
- Free DatabaseTreatment Guides
- Free Lab TestsProduct Lab Tests: Purity & Potency
- Free Video & Write-upEvidence Quality Masterclass
- Free Interactive GuideDermatology Appointment Guide
More
Articles100+ free articles.
-
10 Best Shampoos for Thinning Hair Men
-
Does Semaglutide Cause Hair Loss?
-
Does Dandruff Cause Hair Loss?
-
Topical Finasteride: The Best Dosage for Maximizing Regrowth and Minimizing Side Effects
-
Ulo Review: #1 Customized Hair Loss Treatment in 2026
-
10 Best Hair Loss Treatments for Men
-
Best Minoxidil for Men: Top Picks for 2026
-
Does Ozempic Cause Hair Loss?
PublicationsOur team’s peer-reviewed studies.
- Microneedling and Its Use in Hair Loss Disorders: A Systematic Review
- Use of Botulinum Toxin for Androgenic Alopecia: A Systematic Review
- Conflicting Reports Regarding the Histopathological Features of Androgenic Alopecia
- Self-Assessments of Standardized Scalp Massages for Androgenic Alopecia: Survey Results
- A Hypothetical Pathogenesis Model For Androgenic Alopecia:Clarifying The Dihydrotestosterone Paradox And Rate-Limiting Recovery Factors
Menu- AboutAbout
- Mission Statement
Education. Evidence. Regrowth.
- Team Members
PhD's, resarchers, & consumer advocates.
- Editorial Policy
Discover how we conduct our research.
- Contact
Have questions? Contact us.
- Before-Afters
Before-Afters- Transformation Photos
Our library of before-after photos.
- Client Testimonials
Read the experiences of members
Before-Afters/ Client Testimonials- Popular Treatments
-
ArticlesP. Acnes (Bacteria That Causes Acne) Linked To Hair Loss: What To Do About It
First Published Jun 28 2017Last Updated Sep 19 2025IngredientsMiscellaneous Researched & Written By:Perfect Hair Health Team
Researched & Written By:Perfect Hair Health Team Reviewed By:Rob English, Medical Editor
Reviewed By:Rob English, Medical Editor
Want help with your hair regrowth journey?
Get personalized support, product recommendations, video calls, and more from our researchers, trichologists, and PhD's dedicated to getting you the best possible outcomes.
Learn MoreFull Article
Read time: 15 minutes
Acne, Hair Loss, And The Microbiome
Can the trillions of bacteria living in our gut and skin influence our predisposition to acne and hair loss? Ten years ago, the answer was, “no.” But today researchers are changing their tune.
Evidence shows that the non-human bacteria living in (and on) us — known as our microbiome — helps regulate everything from our moods to our hormones… and maybe even our susceptibility to hair loss.
In fact, a study reveals that a bacterial strain known as propionibacterium acnes — a bacteria commonly associated with acne — may also contribute to a form of hair loss known as diffuse hair thinning.
This article reveals why.
First we’ll dive into the science behind the microbiome: why some bacteria cause infection while others don’t.
Then we’ll uncover the latest research on p. acnes — how this bacteria can trigger an inflammatory response, when p. acnes is associated with acne (and when it’s not), why p. acnes is also linked to hair loss, and whether p. acnes really causes hair loss… or is just an opportunistic invader of another symptom connected to hair thinning.
All-Natural Hair Supplement
The top natural ingredients for hair growth, all in one supplement.
Take the next step in your hair growth journey with a world-class natural supplement. Ingredients, doses, & concentrations built by science.

You might find this article helpful if you’re curious about…
- The connection between our microbiome, acne, and hair loss
- Why your acne blemishes always flare up in the same place, year after year
- Why most antibiotics fail to fight off p. acnes, and how they can increase acne severity in the long-run
- How to stop the over-colonization of p. acnes to reduce acne and keep your health (and hair) in check
Our Microbiome Affects Our Health (And Hair)
Our bodies are colonized by thousands of different microorganisms – bacteria, fungi, viruses, and even parasites. And these bugs are everywhere — from our gastrointestinal tracts to our skin and scalps.
In fact, our bodies are covered in at least as many non-human cells as we have human cells (don’t believe the old saying that we have ten times more bacterial cells than we do humans — those estimates are outdated!).
Many of these microorganisms are harmless. We call these “resident” bugs commensal microorganisms — and by definition, commensal microorganisms don’t cause infection.
Unfortunately, not all microorganisms are commensal. Some bacteria can hurt us — and even kill us.
Why Do Some Microorganisms Cause Infection, While Others Don’t?
It has to do with one thing: whether a bacteria triggers an inflammatory response from our bodies.
Some bacteria exist inside and around us — eating dead cells and partially digested foods. And as long as our bodies don’t perceive these bacteria as threats — we generally leave them alone.
But sometimes our bodies do find a bacteria threatening. This often isn’t the result of the bacteria… but rather, what the bacteria is doing (like eating our living tissues, or even releasing toxic byproducts).
And in order to understand how p. acnes is linked to acne and hair loss, we need to know exactly how “pathogenic” bacteria trigger our bodies into an inflammatory response.
So let’s illustrate this process with a familiar example: the bacteria that causes strep throat.
Example: Streptococcus Pyogenes, Inflammation, And Strep Throat
Strep throat is a bacterial infection in our throats that causes tonsil pain, fever, difficulty swallowing, and significantly swollen throat tissues. Here’s what happens:
Through food or fluid exchanges with an infected person, a bacteria known as streptococcus pyogenes enters our throats and begins competing against our commensal (safe) bacteria for resources — like dead cells and microorganisms. Eventually, streptococcus pyogenes beats out our commensal bacteria. Then it replicates. It rapidly colonizes our throats — reproducing quickly and in high numbers.
The problem: as streptoccocus progenes eats resources, it produces — as a byproduct — toxins. And as the colony grows, this bacteria produces higher levels of toxic byproducts.
By definition, toxins are poisonous. They can’t be easily digested. Some toxins even damage tissues. So in the presence of a toxin overload, our tissues sense cellular damage, and our bodies react by activating certain signaling proteins.
These proteins tell our bodies to begin a pro-inflammatory response — increasing blood flow to the damaged area — so that more blood floods the tissues (and inside that blood, more signaling proteins).
The result: tissue swelling. That painful, sore, difficult-to-swallow aching we get with strep throat.
But ironically, this “swelling” — which most doctors try to reduce — serves three critical purposes:
- The swelling is feedback that our signaling proteins are still at work, and that they’re still needed to repair injured cells, clear away cellular debris, and metabolize any tissues beyond saving. (Healing)
- The swelling clots our blood to prevent the infection from spreading. (Threat Localization)
- This swelling creates an environment where it’s harder for the infectious bacteria to survive. (Adaptive Immune Response)
That third point is important. These signaling proteins don’t just help us heal. They also attack the toxin-releasing bacteria. And if an infection is severe enough, these proteins will even tell our bodies to induce a fever — since many infectious bacteria can’t survive in climates hotter than our normal body temperature.
These “reactions” (which doctors call symptoms) persist until enough streptococcus pyogenes is eliminated and the toxin load reaches a safe level. Then our bodies begin an anti-inflammatory response — where new signaling proteins arrive to tell our tissues to stop swelling and clotting — and that the repairs are finished.
The end-result: the defeat of streptococcus pyogenes, and a resolution of all those painful symptoms.
And that’s how our bodies fight off pathogenic bacteria. We sense a toxin or tissue damage, signal a threat, send blood to the damaged area, clot and swell our tissues, fight the infection, repair the damages, and heal.
And that’s the major difference between pathogenic bacteria and commensal bacteria: pathogenic = inflammation; commensal = little to no inflammation.
Now that we know this, let’s dive into where the bacteria p. acnes comes into play — why it’s so invasive, how it’s linked to both acne and hair loss, and why our bodies have a hard time fighting off overgrowths.
P. Acnes: A Bacteria Linked To Acne & Hair Loss
The bacteria propionibacterium acnes (p. acnes) straddles the line between pathogenic (eliciting an inflammatory response) and commensal (harmless).
On one hand, p. acnes is one of the three major commensal genera that make up our skin microbiome (staphylococcus, corynebacterium, and propionibacterium). Propionibacterium (like p. acnes) are found on skin surfaces and deep within our hair shafts and sebaceous glands. In normal amounts, propionibacterium don’t elicit an inflammatory response.
On the other hand, p. acnes does elicit inflammation if it over-colonizes certain tissues. Specifically, our sebaceous glands (and hair follicles).
In fact, the over-colonization of p. acnes in sebaceous tissues is the connecting point between p. acnes, inflammation and acne (we’ll get to hair loss soon).
How P. Acnes Triggers Acne
Step #1: P. Acnes Colonizes Our Sebaceous Glands
Sebaceous glands are glands within our skin that secrete sebum — an oily bodily lubricant — into our hair follicles.
(source)
Sebum (the oil secreted by the sebaceous gland) lubricates our hair and skin. Sebum helps create a protective barrier between our skin and the rest of the world — specifically, pathogenic microorganisms.
Unfortunately, sebum can’t protect us from all microorganisms. Some microorganisms actually feed off of sebum… P. acnes is one of them.
P. acnes typically colonizes places where sebum production runs rampant — like our faces and hair. That’s why propionibacterium acnes is found in the ducts of our sebaceous glands. It’s as close to its food source (sebum) as it can get.
Unfortunately, this comes with consequences.
Step #2: P. Acnes Feeds Off Sebum And Cellular Debris
Once p. acnes enters the sebaceous gland, it has access to a plentiful supply of sebum and cellular debris. This allows p. acnes to thrive and reproduce freely.
This isn’t necessarily a problem… unless p. acnes grows too large. Why? Because when p. acnes grows, it also releases a number amount of metabolic byproducts, including…
- …more partially digested cellular debris
- …enzymes that break down more sebum (food for p. acnes) — which inadvertently damage the cells inside our sebaceous glands.
The end-result: increased sebum production (to replace the eaten sebum), increased cellular damage, increased cellular debris, and the rapid colonization of p. acnes as its food supply continuously replenishes.
At this point, we have a problem.
Step #3: Our Bodies React By Releasing Signaling Proteins
Similar to how our throats sense the toxic byproducts of streptococcus pyogenes, our sebaceous glands also sense the cellular damage created from p. acnes… and respond by releasing signaling proteins.
Here’s what happens: the skin cells surrounding our sebaceous tissues release pro-inflammatory signaling proteins — specifically, interleukins and tumor necrosis factor. And what do these proteins do?
Step #4: Those Proteins Kickstart An Inflammatory Response
A pro-inflammatory response begins… Our tissues near the sebaceous glands start to swell with blood.
This blood then carries more signaling proteins — which leads to more swelling. And just like the throat swelling with strep throat, sebaceous gland swelling helps us…
- Repair the tissues damaged by p. acnes,
- Kill off the invading bacteria, and…
- Clot our blood — so the “infection” doesn’t spread beyond the sebaceous gland
And what’s a consequence of this inflammatory response?
Step #5: The Inflammation Shows As Acne (Pimples)
That’s right. Acne (and pimples) are as simple as that: they’re a consequence of our body’s inflammatory response. And this inflammatory response is the result of the toxic byproducts produced by high numbers of p. acnes.
In other words, it’s not the p. acnes that causes the pimple… it’s our cells’ reaction to the byproducts of p. acnes that causes the pimple.
And that’s how p. acnes generates inflammation in the upper part of hair follicles — and is linked to acne.
This is also why we don’t get acne where there aren’t sebaceous ducts (and thereby hair follicles). For instance — we don’t get acne on our hands or the bottom of our feet — there are no sebaceous glands. If we do get acne here… it’s probably not acne — and we should go to a doctor.
So knowing this, where does the p. acnes-hair loss connection come into play?
How Is P. Acnes Connected To Hair Loss?
So far, p. acnes is associated with hair loss through…
- The release of molecules known as porphyrins, and…
- A case study analyzing thinning hair shafts and p. acnes infection
Let’s take these one-by-one.
P. Acnes, Porphyrins, Reactive Oxygen Species, & Hair Loss
Porphyrins are molecules produced by our bodies that help support aerobic (oxygen-dependent) life.
You’ve probably heard of the most well-known porphyrin — heme. Heme is responsible for the pigment in our red blood cells, and it’s a cofactor for hemoglobin — a protein that helps carry iron throughout our blood.
P. Acnes Releases Porphyrins
Interestingly, when p. acnes eats sebum inside the sebaceous gland, it also releases porphyrins. These porphyrin molecules are then activated by the sun (UV light) and produce something known as reactive oxygen species (ROS).
Porphyrins Make Reactive Oxygen Species (ROS)
Reactive oxygen species are oxygen-containing molecules that are so unstable, they need to immediately bind to nearby molecules. Unfortunately, when reactive oxygen species bind to these molecules, it often comes at a cost: the destabilization of enzymes and even cellular degradation. The end-result: inflammation.
Porphyrins & Reactive Oxygen Species (ROS) Are Linked To Pattern Hair Loss
Interestingly, porphyrins in the sebaceous canal are associated with pattern hair loss. In other words, this suggests pattern hair loss may be the result of long-standing inflammation.
But the more pertinent implication? Our bacteria inside the sebaceous canals — like p. acnes — increase porphyrins, ROS, and inflammation — which may contribute to the hair loss cascade.
So goes the p. acnes-porphyrin-hair loss connection… And now, two case studies may further solidify the case that p. acnes contributes to hair loss.
Case Study #1: P. Acnes In Thinning Hair Shafts
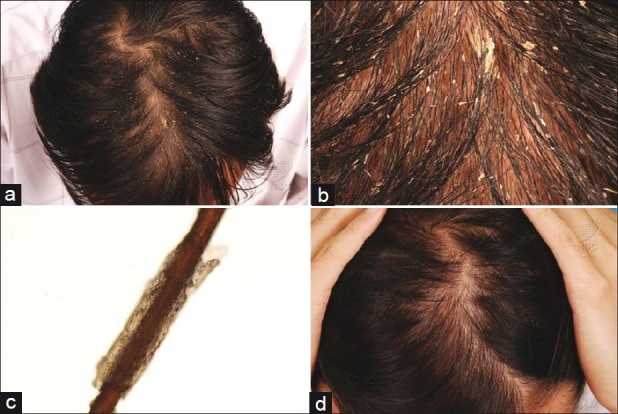
In 2012, A team of researchers evaluated four patients with non-scarring diffuse hair loss — with hair loss ranging from the typical “even” thinning in women… to the patchy hair loss in those with alopecia areata.
In addition to these patients’ thinning hair, each subject also suffered from “hair casts” — a condition characterized by dandruff-like casts encircling the hair shafts.
The investigators decided to take biopsies of the subjects’ hair follicles.
And what did they find?
Isolates of the bacteria p. acnes.
Or in other words, over-colonizations of the same bacteria that produce porphyrins, eat sebum, and cause an inflammatory cascade that results in acne.
Treatment Attempt #1: Anti-Dandruff Creams
The researchers attempted to treat the patients with standard anti-dandruff shampoos — but the hair casts (and hair loss) persisted.
Treatment Attempt #2: Antibiotics For P. Acnes
Then the subjects began a round of systemic antibiotics to target the p. acnes infection.
Within weeks, the hair casts disappeared. In addition, the patients reported either a slowing of hair loss, a stop in hair loss, or in one case — even hair regrowth (when combined with minoxidil).
Results: Hair Casts Disappear; Hair Loss Stops
Unfortunately, no hair count analyses were performed. Each patient’s hair growth was either self-reported or determined during a follow-up examination. So it’s tough to say just how much the removal of these hair casts (and thereby a reduction in p. acnes) helped with hair regrowth.
In any case, the clearance of hair casts are evident in the photos:
(a) and (b) show a patient with hair casts and diffuse hair loss; (c) shows a hair cast under a microscope; (d) shows clearance of the hair casts after treatment with antibiotics against p. acnes. (source)
The case study is interesting, but without more data, we can’t draw conclusions and say that p. acnes was the cause of hair loss for these patients…
…but the research implicating p. acnes in hair loss continues to grow — especially in the next case study.
Case Study #2: Calcification & P. Acnes
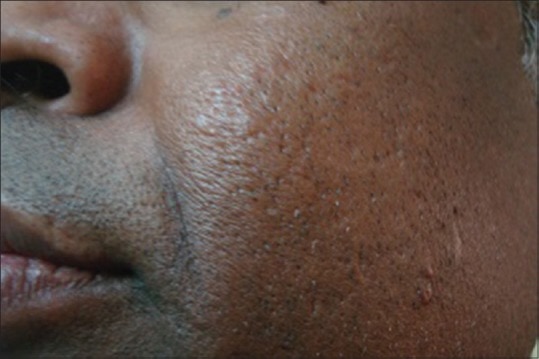
These researchers published a study of a patient with acne scars and a condition known as calcinosis cutis.
Calcinosis cutis is the abnormal deposition of insoluble calcium in and under the skin. And despite its brutal-sounding name, typically this calcification (and scarring) isn’t too visible on the skin surface.
Just look at this photo. Despite teenage (and adult) acne, the patient’s skin has relatively little scarring…
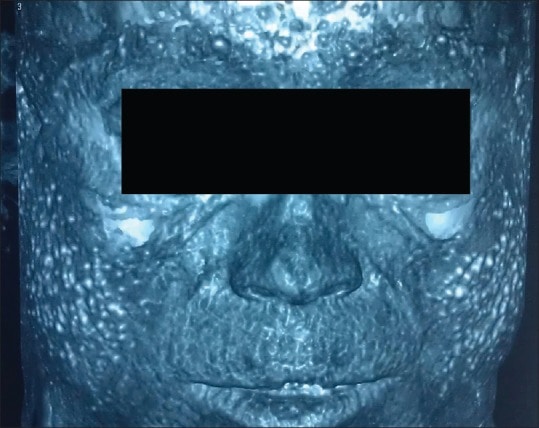
Unfortunately, this photo doesn’t show the full picture of soft tissue calcification. Because when researchers did a tomography scan for soft tissue calcification, here’s what they discovered:
Those white dots are all signs of soft tissue calcification. And that calcification is far more prevalent than what we see at the skin surface. In fact, this soft tissue calcification appears to have deposited in major acne sites — or in other words, places of inflammation likely triggered by p. acnes.
How Is Calcification Relevant To P. Acnes?
For one, p. acnes is a causative factor in acne. And this case study demonstrates that for some individuals, acne may result in soft tissue calcification deposits within our sebaceous glands.
That means we need to study the implication that p. acnes might also play some sort of role in this soft tissue calcification — and whether this soft tissue calcification is the difference between scarring and non-scarring acne.
Now, calcification might not be a widespread phenomenon for most acne sufferers… but we don’t yet know. To my knowledge, most acne sufferers aren’t lining up for facial tomography scans. And the reality is — soft tissue calcification might occur in a majority of those with acne… But we haven’t yet done the studies.
And without these studies, we can’t rule out that p. acnes might play some causal role in hair loss.
How Are Calcification, P. Acnes, And Hair Loss Connected?
Well, p. acnes doesn’t just live on our skin. P. acnes is also found in our arteries. And interestingly, p. acnes in our blood capillaries is associated with atherosclerosis (the hardening of arteries), which may lead to calcium deposits inside our arteries.
In balding men, calcification is also found in the blood capillaries supporting thinning hair follicles (but not in non-thinning hair follicles). In fact, this observation was first made in the 1920’s!
There’s also growing evidence that calcification precedes pattern hair loss, and that calcification might even be a consequence of elevated DHT (the hormone commonly associated with pattern hair loss).
The bottom line: we need to explore the relationship between p. acnes, inflammation, calcification, and hair loss further. But for now, all we know is that p. acnes can increase inflammation in the sebaceous gland, and that for some individuals, this inflammation may lead to soft tissue calcification.
Can We Reduce P. Acnes To Fight Acne (And Maybe Even Hair Loss)?
There are no easy answers here. But first, let’s start off with what not to do when suffering from p. acnes over-colonization (and thereby acne and potentially hair loss).
Conventional Treatments Fail To Reduce P. Acnes Effectively
Here’s how I define an “effective treatment”:
- The treatment must reduce p. acnes colonization (and thereby acne)
- The treatment must not lead to major unintended consequences to our health
Unfortunately, most conventional treatments fail on both categories. Here are two examples:
Failure #1: Antibiotics For P. Acnes
Systemic (oral) antibiotics are moderately effective at reducing p. acnes infection. In fact, this is why many doctors prescribe low-grade antibiotics like amoxycillin to fight off acne.
The good news is that during treatment, acne typically does reduce (and even go away completely).
But this comes with consequence. The problem is that p. acnes is everywhere. It recolonizes quickly after a round of antibiotics. And the p. acnes that survives antibiotic treatment typically builds a resistance to that antibiotic.
Problem #1: P. Acnes Becomes Antibiotic-Resistant
This is a bigger issue than most medical practitioners recognize. In fact, p. acnes resistance to antibiotics has grown from ~20% in the 1970’s to ~60% in the 1990’s — with new estimates suggesting as much as 80% of p. acnes are resistant to standard antibiotic treatment today!
Problem #2: This May Cause Recurring Acne Lesions From P. Acnes (Repeat Blemishes!)
The second issue is that once this antibiotic-resistant p. acnes recolonizes our sebaceous glands, it evokes the same inflammatory response: acne. Only this time, we can’t use antibiotics to treat it.
In fact, this is why so many people end up getting the same blemishes, in the same place, year after year. This type of acne recurrence is more typical in acne sufferers who have been treated with antiobiotics in the past! It’s the same p. acnes colony in the same sebaceous glands — overgrowing again and again.
Problem #3: Systemic Antibiotics Inadvertently Kill Other Bacteria — And Even Bacteria We May Need For Healthy Functionality
Research now reveals that certain microorganisms aren’t all bad. In fact, some bacteria even create symbiotic relationships with our bodies — increasing vitamin metabolism, dampening overactive immune responses, and even helping regulate hormone secretion, cognitive function, and even our responses to stress and anxiety.
Unfortunately, antibiotics don’t discriminate the bad from the good bacteria. They wipe out everything. And when it comes time to recolonize, you’re literally rolling the dice and hoping good bacteria will recolonize instead of bad bacteria.
Sadly, the dice often rolls against your favor. For instance, antibiotic abuse is now linked to the resurgence of a bacteria known as clostridium difficile, which killed 29,000 Americans in 2011. That’s over three times as many American deaths than the HIV/AIDS virus for the same year.
The bottom line: think twice about antibiotic use. It’s a short-term win with long-term consequences.
Failure #2: Accutane For P. Acnes
Accutane is the brandname of a drug known as isotretinoin — which is a synthetic derivative of a retinoid (or in other words, the animal form of vitamin A). Essentially, it’s similar to high oral doses of retinol (vitamin A).
Accutane (Isotretinoin) is extremely effective at reducing moderate-to-severe acne — even after treatment is stopped. Why? Because Accutane atrophies (and can even destroy) our skin’s sebaceous glands.
This reduces sebaceous gland functionality, which reduces sebum production. P. acnes eats sebum to survive. And with less sebum production, p. acnes has less food. That makes it more difficult for p. acnes to colonize (or over-colonize) a sebaceous gland — because there’s significantly less food for them.
The end-result: Accutane significantly reduces p. acnes colonization in the skin and in hair follicle ducts. And in doing so, it reduces sebaceous gland inflammation… and thereby reduces acne.
The good news: Accutane irreversibly atrophies our sebaceous glands, so that p. acnes colonization and acne lesions decrease for life.
The bad news: Accutane irreversibly atrophies our sebaceous glands, and is extremely toxic.
Side Effects Of Accutane Use: Depression, Autoimmune Disease, Liver Damage, And Pancreatitis
Properly diving into the dangers of Accutane would turn this 4,000 word article into a book. But the bottom line is this: Accutane is a synthetic derivative of retinol, and high dosages, retinol is extremely toxic.
Problem #1: Retinol Toxicity
In fact, retinol toxicity — or hypervitaminosis A — is why you should never eat polar bear liver. It’s extremely high in retinol, and our bodies can’t metabolize surging amounts of retinol all at once. If we try, our livers and pancreas will likely shut down.
Problem #2: Accutane Decreases Brain Activity In The Frontal Cortex
Accutane is synthetic — meaning it is a chemical derivative that mimics the look of natural-occurring retinoids. Our bodies don’t always read synthetic chemicals the same way they do their naturally-occurring molecular counterparts. And this “difference” tends to play out in Accutane’s effects on brain activity.
In fact, one study suggests that Accutane users experienced a 21% decrease in brain metabolism in the orbito-frontal cortex. This partly explains why Accutane users have to be monitored closely for depression and suicidal thoughts.
Problem #3: Accutane May Be A Trigger To Autoimmune Thyroid Disease
Accutane is also linked to increased incidences of irritable bowel syndrome and Crohn’s disease. With that said, the scientific consensus on association versus causation is still up for debate — and without a clear mechanism action, we can’t make any major claims.
However, Isotretinoin drugs (like Accutane) may also play a role in the development of autoimmune-based thyroid disease — at least according to this case study. But evidence here is still being explored.
Problem #4: Accutane Has Already Been Discontinued (But Not Really)
Since 2009, the brandname Accutane is no longer available as an acne treatment. This is the result of a series of class action lawsuits and litigation troubles for the drug maker, Roche USA.
But that doesn’t mean you still can’t get Accutane. In fact, Accutane is just one brand name for the drug isotretinoin. Isotretinoin is still available as a generic drug — and now comes packages as several other brand names.
So if you’re suffering from a p. acnes overgrowth and have acne (and maybe even hair loss), what should you do?
How To Fight P. Acnes Effectively (Without Drugs)
When it comes to fighting p. acnes — and fighting hair loss, too — there’s no “one size fits all” answer.
The causes of the p. acnes overgrowths are complex and multifaceted. As such, the treatments are complicated too. But if you’re suffering from acne (and maybe even hair loss), here are some good starting places.
Treatment #1: Eliminate Small Intestinal Bacterial Overgrowth
Our small intestines are used for nutrient absorption and are typically absent of large amounts of bacteria. However, psychological stress, a poor diet, and lacking sleep (among other triggers) can often lead to a condition known as Small Intestinal Bacterial Overgrowth (SIBO).
Small intestinal bacterial overgrowth (SIBO) is when bacterial colonies overgrow in the small intestine — which is typically devoid of significant amounts of bacteria and microorganisms. This leads to nutrient malabsorption and a host of other symptoms — from depression to acne and maybe even hair loss (expect an article on this soon).
Interestingly, people with acne rosacea are ten times more likely to suffer from SIBO than those without acne. In fact, practitioners who have successfully treated SIBO (like Chris Kresser) have stated that nearly 100% of the patients they treat for acne also test positive for SIBO.
Encouragingly, of the patients who are successfully treated for SIBO, their acne almost always disappears.
In fact, treating SIBO is my number one recommendation for reducing p. acnes overgrowths and eliminating acne (and possibly eliminating p. acnes as a hair loss trigger). If you prioritize any acne treatment, prioritize getting checked for SIBO, and then treating it effectively.
How To Test For (And Treat) Small Intestinal Bacterial Overgrowth
If you don’t have access to medical professionals who routinely treat complex cases of small intestinal bacterial overgrowth — like Chris Kresser or Dr. Amy Nett — I’d recommend you try following a protocol that’s proven successful (repeated times) for other individuals.
John Brisson of fixyourgut.com has had success treating many individuals with SIBO. In fact, I was referred to his work by a readers of this site who used John’s protocol to resolve his own SIBO symptoms. I respect John’s research and have no issues recommending him.
If you do attempt one of his protocols (which are published online for free), be sure you’ve properly diagnosed your type of SIBO. Testing information can also be found on his site.
Treatment #2: Reduce Sebum Production
Accutane is a drug that successfully reduces sebum production, but at the cost of unintended side effects. Is there a way to reduce excess sebum production without the use of isotretinoin drugs?
Yes. Let’s explore a few ways researchers are trying to do this.
#1: Topical Drugs That Reduce Sebum Production: Olumacostat Glasaretil
Olumacostat glasaretil (OG) is a drug that targets to reduce moderate-to-severe acne. It’s currently in human trials, and if approved, it’ll be the only acne-treatment drug that works exclusively by reducing sebum production.
OG is topically applied and works by inhibiting an enzyme called acetyl coenzyme-A carboxylase — which is needed to synthesize the fatty acids inside sebum. With less acetyl coenzyme-A carboxylase present, less sebum fatty acids are secreted to the skin, and thereby fewer p. acnes can colonize that skin.
Studies show that Olumacostat glasaretil significantly reduces sebum production and shows promise as an acne-treatment topical. The question remains: will it survive human trials without significant side effects? We won’t know for many months — but given acetyl coenzyme-A carboxylase’s importance in other organs of the body (like our livers) — the severity of side effects will probably depend on how much topically OG is systemically absorbed. For reference — I would never take this drug orally.
#2: Change Your Diet
Studies now demonstrate that sebum production is highly dependent on diet.
For instance, some studies show a strong correlation between excessive sebum production and carbohydrate-heavy westernized diets. Other studies speculate that high fat consumption — especially oxidized polyunsaturated fats — may also be linked to acne.
Which Diet Should You Try?
The reality is — I can’t tell you. Our microbiomes all vary. As such, each person’s system is going to respond differently to any particular diet. For reference, I had increased acne on a Standard American Diet, and persistent acne (and hair loss) while experimenting on a vegetarian (and then vegan) diet.
Ironically, I experienced increased sebum production on a low-carb paleo diet… but a significant reduction in acne. For the last few years I’ve been experimenting with a moderate carbohydrate paleo-based diet — which appears to be the best for me in terms of a cessation in hair loss, but I still get a little acne from time-to-time.
The bottom line is that you should start testing. A paleo-based model (with modifications) is currently what I’m following — and with success. But that doesn’t mean it will be the best solution for you.
Eat More (Unoxidized) Linoleic Acid
Sebum from acne-bearing skin appears to have less linoleic acid — a fatty acid from the omega 6 family. Linoleic acid is an essential fatty acid — which means our bodies can’t produce it on its own. So if you’re suffering from acne, you might want to consider getting more linoleic acid into your diet.
Sources include pumpkin seed oil and most nuts (though eat these sparingly and away from meals — as the lectin and phytate content in nuts can decrease total nutrient absorption). And above all, make sure any linoleic acid you consume is unoxidized.
Eat More Retinol (Vitamin A) — Just Not From Polar Bears
Accutane’s science was built off the fact that retinol (vitamin A from animal sources) modifies sebaceous gland structure and sebum secretion. A great way to reduce sebum production is simply to eat more retinol. Sources include ground beef, liver, and most organ meats.
Decrease Your Consumption Of Iron-Rich Foods (Or Donate Blood)
While it might seem at odds with the recommendation above (as liver is very iron-rich),
Studies show that p. acnes enzyme activity (the byproducts which p. acnes releases that damage our cells) increases in the presence of iron. In fact, this partially explains why p. acnes in our blood stream is so dangerous — because the availability of iron in our blood increases these p. acnes enzymes, which increases porphyrins, which increases ROS, which leads to inflammation, which leads to atherosclerosis.
To combat the proliferation of p. acnes in our blood, we should…
- Decrease our consumption of iron-heavy foods
- Pair our consumption of iron-heavy foods with iron binders (like calcium or caffeine)
- Donate blood
All three of these strategies should help with iron depletion, and in doing so, lower oxidative stress, decrease p. acnes in the blood, and prevent arterial plaque build-up. In fact, researchers think that isotretinoin’s effects on bacterial iron metabolism may be why the drug atrophies sebaceous glands and decreases sebum production. So it’s not too farfetched to suggest that decreasing iron in the blood might improve our skin quality overall.
Treatment #3: Probiotics (And Other Microorganisms)
While many studies suggest that probiotics can exacerbate acne (likely as a result of increased SIBO), new research demonstrates that certain microorganisms directly compete with p. acnes to keep any overgrowths at bay.
In fact, a commensal skin bacteria known as staphylococcus epidermidis directly inhibits the growth of p. acnes. This is a new discovery, and a very exciting one.
The implication is that a simple probiotic topical (of s. epidermidis) might resolve long-standing acne lesions… without disrupting the rest of our microbiome. That means a resolution in acne, and no side effects.
If more studies confirm these findings, it’s likely that a fermented s. epidermidis topical will make it to market as an acne treatment — and will be much safer versus drugs and antibiotics.
Final Thoughts
The bacteria p. acnes is directly implicated as a cause of acne… and is present in the hair shafts of some men and women with thinning hair. While p. acnes isn’t yet implicated as a cause of hair loss, it may contribute to pattern hair loss through the release of porphyrins and its potential connection to soft tissue calcification.
P. acnes isn’t necessarily a problem until the bacteria is 1) in our blood stream, or 2) overgrown in our sebaceous gland tissues. In my experience, the number one way to eliminate p. acnes overgrowth in either our skin or blood is to test for (and treat) small intestinal bacterial overgrowth.
Secondary measures to reducing p. acnes overgrowths include experimenting with our diets, reducing iron overload, and maybe even testing topical probiotics containing specific strands of s. epidermidis. All of these treatment options should help reduce p. acnes proliferation, inflammation, acne, and indirectly maybe even hair loss (though don’t get your hopes up on a hair recovery from eliminating p. acnes only).
Above all, don’t resort to antibiotic treatments or isotretinoin drugs to reduce acne. The long-term consequences far outweigh the short-term benefits.
Want help with your hair regrowth journey?
Get personalized support, product recommendations, video calls, and more from our researchers, trichologists, and PhD's dedicated to getting you the best possible outcomes.
Learn More
Perfect Hair Health Team
"... Can’t thank @Rob (PHH) and @sanderson17 enough for allowing me to understand a bit what was going on with me and why all these [things were] happening ... "
— RDB, 35, New York, U.S.A."... There is a lot improvement that I am seeing and my scalp feel alive nowadays... Thanks everyone. "
— Aayush, 20’s, Boston, MA"... I can say that my hair volume/thickness is about 30% more than it was when I first started."
— Douglas, 50’s, Montréal, CanadaWant help with your hair regrowth journey?
Get personalized support, product recommendations, video calls, and more from our researchers, trichologists, and PhD's dedicated to getting you the best possible outcomes.
Join Now - Mission Statement
 Scroll Down
Scroll Down