- About
- Mission Statement
Education. Evidence. Regrowth.
- Education.
Prioritize knowledge. Make better choices.
- Evidence.
Sort good studies from the bad.
- Regrowth.
Get bigger hair gains.
Team MembersPhD's, resarchers, & consumer advocates.
- Rob English
Founder, researcher, & consumer advocate
- Research Team
Our team of PhD’s, researchers, & more
Editorial PolicyDiscover how we conduct our research.
ContactHave questions? Contact us.
Before-Afters- Transformation Photos
Our library of before-after photos.
- — Jenna, 31, U.S.A.
I have attached my before and afters of my progress since joining this group...
- — Tom, 30, U.K.
I’m convinced I’ve recovered to probably the hairline I had 3 years ago. Super stoked…
- — Rabih, 30’s, U.S.A.
My friends actually told me, “Your hairline improved. Your hair looks thicker...
- — RDB, 35, New York, U.S.A.
I also feel my hair has a different texture to it now…
- — Aayush, 20’s, Boston, MA
Firstly thank you for your work in this field. I am immensely grateful that...
- — Ben M., U.S.A
I just wanted to thank you for all your research, for introducing me to this method...
- — Raul, 50, Spain
To be honest I am having fun with all this and I still don’t know how much...
- — Lisa, 52, U.S.
I see a massive amount of regrowth that is all less than about 8 cm long...
Client Testimonials150+ member experiences.
Scroll Down
Popular Treatments- Treatments
Popular treatments. But do they work?
- Finasteride
- Oral
- Topical
- Dutasteride
- Oral
- Topical
- Mesotherapy
- Minoxidil
- Oral
- Topical
- Ketoconazole
- Shampoo
- Topical
- Low-Level Laser Therapy
- Therapy
- Microneedling
- Therapy
- Platelet-Rich Plasma Therapy (PRP)
- Therapy
- Scalp Massages
- Therapy
More
IngredientsTop-selling ingredients, quantified.
- Saw Palmetto
- Redensyl
- Melatonin
- Caffeine
- Biotin
- Rosemary Oil
- Lilac Stem Cells
- Hydrolyzed Wheat Protein
- Sodium Lauryl Sulfate
More
ProductsThe truth about hair loss "best sellers".
- Minoxidil Tablets
Xyon Health
- Finasteride
Strut Health
- Hair Growth Supplements
Happy Head
- REVITA Tablets for Hair Growth Support
DS Laboratories
- FoliGROWTH Ultimate Hair Neutraceutical
Advanced Trichology
- Enhance Hair Density Serum
Fully Vital
- Topical Finasteride and Minoxidil
Xyon Health
- HairOmega Foaming Hair Growth Serum
DrFormulas
- Bio-Cleansing Shampoo
Revivogen MD
more
Key MetricsStandardized rubrics to evaluate all treatments.
- Evidence Quality
Is this treatment well studied?
- Regrowth Potential
How much regrowth can you expect?
- Long-Term Viability
Is this treatment safe & sustainable?
Free Research- Free Resources
Apps, tools, guides, freebies, & more.
- Free CalculatorTopical Finasteride Calculator
- Free Interactive GuideInteractive Guide: What Causes Hair Loss?
- Free ResourceFree Guide: Standardized Scalp Massages
- Free Course7-Day Hair Loss Email Course
- Free DatabaseIngredients Database
- Free Interactive GuideInteractive Guide: Hair Loss Disorders
- Free DatabaseTreatment Guides
- Free Lab TestsProduct Lab Tests: Purity & Potency
- Free Video & Write-upEvidence Quality Masterclass
- Free Interactive GuideDermatology Appointment Guide
More
Articles100+ free articles.
-
Does Dandruff Cause Hair Loss?
-
Topical Finasteride: The Best Dosage for Maximizing Regrowth and Minimizing Side Effects
-
Ulo Review: #1 Customized Hair Loss Treatment in 2026
-
10 Best Hair Loss Treatments for Men
-
Best Minoxidil for Men: Top Picks for 2026
-
Does Ozempic Cause Hair Loss?
-
Does Masturbation Cause Hair Loss?
-
6 Best Hair Loss Treatments for Women
PublicationsOur team’s peer-reviewed studies.
- Microneedling and Its Use in Hair Loss Disorders: A Systematic Review
- Use of Botulinum Toxin for Androgenic Alopecia: A Systematic Review
- Conflicting Reports Regarding the Histopathological Features of Androgenic Alopecia
- Self-Assessments of Standardized Scalp Massages for Androgenic Alopecia: Survey Results
- A Hypothetical Pathogenesis Model For Androgenic Alopecia:Clarifying The Dihydrotestosterone Paradox And Rate-Limiting Recovery Factors
Menu- AboutAbout
- Mission Statement
Education. Evidence. Regrowth.
- Team Members
PhD's, resarchers, & consumer advocates.
- Editorial Policy
Discover how we conduct our research.
- Contact
Have questions? Contact us.
- Before-Afters
Before-Afters- Transformation Photos
Our library of before-after photos.
- Client Testimonials
Read the experiences of members
Before-Afters/ Client Testimonials- Popular Treatments
-
ArticlesIodine For Hair Loss? Think Twice About Supplementing
First Published Jul 9 2020Last Updated Sep 19 2025IngredientsNatural Remedies Researched & Written By:Perfect Hair Health Team
Researched & Written By:Perfect Hair Health Team Reviewed By:Rob English, Medical Editor
Reviewed By:Rob English, Medical Editor
Want help with your hair regrowth journey?
Get personalized support, product recommendations, video calls, and more from our researchers, trichologists, and PhD's dedicated to getting you the best possible outcomes.
Learn MoreArticle Summary
Less than 10% of Americans are iodine deficient, and even fewer have a hair loss disorder caused by low iodine intake. Ironically, iodine is a trace element featured in many top-selling hair loss supplements, allegedly to help support the thyroid. This article separates fact versus fiction about iodine, its role in hair loss and hair growth, and why people with hypothyroidism (and hair loss) should think twice about supplementing.
Full Article
An Investigation: Iodine & Hair Health
Iodine is a mineral featured in many top-selling hair loss supplements. The rationale for its inclusion? That iodine is an essential nutrient for thyroid function. And, since thyroid disorders are linked to hair loss, iodine must also be critical for hair growth.
There is some truth to this claim. At the same time, this truth is all context specific.
For instance, many people don’t know that iodine supplements are only appropriate for a small percentage of hair loss sufferers. Moreover, there are cases where iodine supplementation may actually cause hair loss.
To understand why, we’ll need to uncover:
- The science behind iodine: what it is, its effects on the thyroid, and its role in hair loss and hair growth.
- The percent of hair loss sufferers who are iodine deficient.
- The scenarios in which iodine will help or hurt or hair.
This article unpacks the evidence, the answers, and more.
All-Natural Hair Supplement
The top natural ingredients for hair growth, all in one supplement.
Take the next step in your hair growth journey with a world-class natural supplement. Ingredients, doses, & concentrations built by science.

What is iodine?
Iodine is an essential mineral found in fish, kelp, dairy products, and (in many countries) salt. It plays crucial roles in the maintenance of brain, thyroid, and metabolic health. It’s especially important for the growth and development of fetuses and children.
Iodine: an essential trace element
In 1990, almost one-third of the global population was affected by iodine deficiency, making it the single greatest preventable cause of brain damage. As such, salt iodization programs were initiated at the national level, leading to a drastic decline in the incidence of iodine deficiency. Today, only 8.8% of people in the U.S. are considered iodine deficient.
So, who are these individuals who are iodine deficient or at risk of a deficiency? And are these deficiencies linked to hair loss?
To answer these questions, we’ll first unpack the evidence on iodine and hair loss. Then, we’ll establish when iodine deficiencies are connected to hair loss (and when they aren’t).
Finally, we’ll reveal evidence for why people should think twice about taking iodine for hair health. After all, there’s evidence that iodine supplementation can hurt our thyroid, too… and maybe even our hair.
Is there any evidence that iodine plays a role in hair growth or hair loss?
Yes. Evidence from human and animal studies suggests that iodine deficiencies may contribute to hair health, and in a few ways:
- Thyroid hormones are essential for maintaining the growth of hair. This is why hypothyroidism, a state of low thyroid hormone, is directly connected to hair loss. Iodine is essential for the creation of thyroid hormones and, thus, deficiency may limit thyroid hormone synthesis. Hypothyroidism is mostly linked to telogen effluvium, a hair shedding disorder that leads to non-permanent diffuse hair loss. But it has also been linked to female androgenic alopecia (AGA).
- Thyroid hormones have been shown to reduce skin fibrosis in animal studies. Thyroid hormones may, therefore, limit (but not necessarily fully block) fibrosis that contributes to follicle miniaturization in AGA.
So, iodine might affect hair growth… primarily due to its role in thyroid hormone production. To recap: without enough iodine, the thyroid can’t function properly, which can lead to hypothyroidism (an under-active thyroid). And when hypothyroidism is severe enough, hair loss can occur… specifically in the form of telogen effluvium and/or (maybe) female pattern hair loss.
So, can an iodine deficiency cause hair loss?
It’s possible. After all, iodine deficiencies can lead to hypothyroidism, and hypothyroidism can lead to telogen effluvium and/or exacerbate female pattern hair loss.
But just because iodine deficiencies may cause hair loss in certain scenarios does not mean you should supplement with iodine. Why? Because the scenarios we’ve outlined above are relatively uncommon… especially in the developed world.
Consider the following:
- Only 8.8% of Americans are deficient in iodine.
- Only 3-15% of adults in America or the U.K. have subclinical hypothyroidism (source).
Moreover, hypothyroidism can stem from many different causes – i.e., autoimmune disorders, chronic conditions, nutrient deficiencies from zinc and iodine, and more.
That means that only a fraction of the 3-15% of adults with hypothyroidism have hypothyroidism due to an iodine deficiency.
In other words, the percentage of American adults who might benefit from iodine supplementation is 8.8%… and the percentage of American or U.K. adults who might see hair regrowth from iodine supplements is much less than 8.8%.
This means that iodine supplementation is unlikely to help the majority of hair loss sufferers in the developed world. In fact, there are even scenarios where supplementing with iodine might be dangerous, or maybe even cause hair loss.
Here’s how.
Iodine helps the thyroid but, paradoxically, may induce hypothyroidism
Following the iodization of salts, the U.S. and other countries began to see a decrease in the prevalence of goiters – large growths on the neck which are often indicative of hypothyroidism. This, along with the evidence of decreased (preventable) brain damage all pointed to the fact that widespread iodization was working; it was preventing preventable diseases and making people healthier. Moreover, for most people, it seemed like the increased iodine consumption was generally well tolerated. These are all positives.
However, there’s always two sides to every story.
For instance, this meta-analysis of 50 studies revealed that yes, iodization (i.e., widespread iodine supplementation through salts) did decrease the number of goiters. But interestingly, chronic exposure of iodine also increased the incidence of hypothyroidism – mostly in places that were otherwise getting enough iodine to begin with.
This implies that iodine’s effects on thyroid health is biphasic. In other words, both low iodine and high iodine intake can lead to hypothyroidism. Therefore, we shouldn’t shoot to consume as much as possible; we should shoot to consume the optimal amount daily (more on this later).
Iodine helps the thyroid but, paradoxically, may induce hyperthyroidism
Hyperthyroidism is the opposite of hypothroidism; it’s when the thyroid is over-active. And interestingly, hyperthyroidism (like hypothyroidism) is also linked to hair loss, but through a different set of mechanisms.
Whereas hypothyroidism may evoke hair shedding as a result of “metabolic conservation”, hyperthyroidism exposes our hair follicles to too much thyroid hormone – which may deplete hair follicle stem cells (i.e., cells that are necessary for hair growth).
Interestingly, hyperthyroidism is also (paradoxically) sometimes linked to excess iodine intake.
This phenomenon was first observed after the implementation of universal iodization programs. Researchers found that the incidence of hyperthyroidism began to increase in various countries. In some cases, these increases occurred directly alongside increases in salt iodization, suggesting a direct relationship.
Some evidence suggests that hyperthyroidism from excess iodine may also be due to too large of a jump in iodine intake, too quickly. In other words, it seems more prevalent in those jumping from extremely low iodine intake to extremely high iodine intake – which is really only possible through supplementation.
As such, it’s best to fully understand your iodine needs – and your own intake – before considering supplementing.
Any other health concerns with iodine supplementation?
Yes, primarily thyroid cancer.
Studies on populations in Iceland, Hawaii, and China have indicated that increased iodine intake may be a factor in some forms of thyroid cancer. At the same time, the body of research suggests yet another biphasic effect of iodine: low levels of iodine are also a risk factor for thyroid cancers.
So, it appears that both high and low intakes of iodine are implicated in cancer. Again, all roads lead to optimal iodine intake… not deficiencies or excesses.
How severe would an iodine deficiency need to be to cause hair loss?
For hypothyroidism to occur and thereby lead to telogen effluvium-related hair loss, one would have to consume less than 10-20 mcg of iodine per day. This is less than 15% of the recommended daily intake for adults.
For reference, just a quarter teaspoon of iodized salt contains 71 mcg – a quantity high enough to prevent iodine deficiency-related hypothyroidism. But, even for those who don’t consume iodized salt, one egg alone contains 24 mcg. And in most cases, one egg daily would be sufficient to prevent hypothyroidism, and thereby hypothyroid-related hair shedding.
Thus, most cases of hypothyroidism-induced hair loss are likely not attributed to iodine deficiency..
What might interfere with the thyroid’s ability to use iodine?
Beyond iodine consumption, there are some additional factors that can influence the thyroid’s ability to utilize iodine:
- Fluoride. Fluoride has been shown to impair iodine transport and absorption, which impairs thyroidal access to iodine.
- Goitrogens. Goitrogens are compounds found in cruciferous vegetables, legumes, cabbage, kale, cauliflower, broccoli, turnips, and canola. These compounds compete for iodine uptake in the thyroid, thereby displacing active iodine for thyroid hormone synthesis.
But, how likely is it that our fluoride and goitrogen exposure actually influences hypothyroidism?
Some animal studies indicate that goitrogen consumption may impair thyroid function even in the presence of adequate iodine consumption. However, the general consensus is that goitrogens in normal quantities are unlikely to induce hypothyroidism in the presence of optimal iodine intake.
In regards to fluoride, it only appears to be an issue in the case of moderate to severe iodine deficiency. So, again, the risk profiles here are all relative… and relatively small.
How can we safely maintain iodine levels?
A balanced diet with plenty of high-quality plant and animal foods is more than likely to provide all the iodine you need for sufficiency.
However, if you’re concerned that maybe your diet is slightly devoid of iodine, here are some foods you may consider adding to your diet:
Foods and their respective iodine content
Iodized salt (¼ tsp) 71 mcg (47% DV) Seaweed (1g) 16-2,984 mcg (11%-1,989% DV) Cod (3 oz) 99 mcg (66% DV) Low-fat yogurt (1 cup) 75 mcg (50% DV) Reduced fat milk (1 cup) 56 mcg (37% DV) Eggs (1 egg) 24 mcg (16% DV) Beyond that, avoiding iodine in your supplements is probably a good idea.
Iodine is readily accessible and abundant in foods – at least foods available in the developed world. Therefore, supplementation isn’t going to confer many benefits, as only 8.8% of people even have a gap to fill (which can be filled by changing your diet).
Moreover, since iodine supplementation increases the risk of excess intake, this might elevate our risk of thyroid-related problems and, by association, our hair loss. Therefore, iodine supplementation runs the risk of sabotaging our efforts to regrow hair.
In light of this evidence, we’ve never understood why so many hair loss companies are hellbent on including iodine in their supplement line.
For peace of mind, you may also want to reduce your exposure to goitrogens and fluoride by (1) cooking your cruciferous vegetables and (2) filtering your drinking water with a fluoride-removing filter. This should dramatically reduce your exposure to compounds that can interfere with iodine bioavailability.
Aside from that, the evidence suggests that iodine is worth getting from food sources and iodized salt rather than a hair loss supplement. So, if you see a supplement with iodine, and you don’t have hypothyroid-related hair loss due to an iodine deficiency… maybe keep shopping.
Summary
Iodine is essential trace element. It helps support kidney, skin, brain, and thyroid health – and it’s also to help produce thyroid hormones.
Iodization programs have drastically reduced the incidence of iodine deficiencies globally. According to the latest estimates, only 8.8% of Americans have an iodine deficiency. And since both an iodine deficiency as well as iodine excess can cause thyroid-related problems, most Americans (and others in developed countries) should be avoiding iodine supplements.
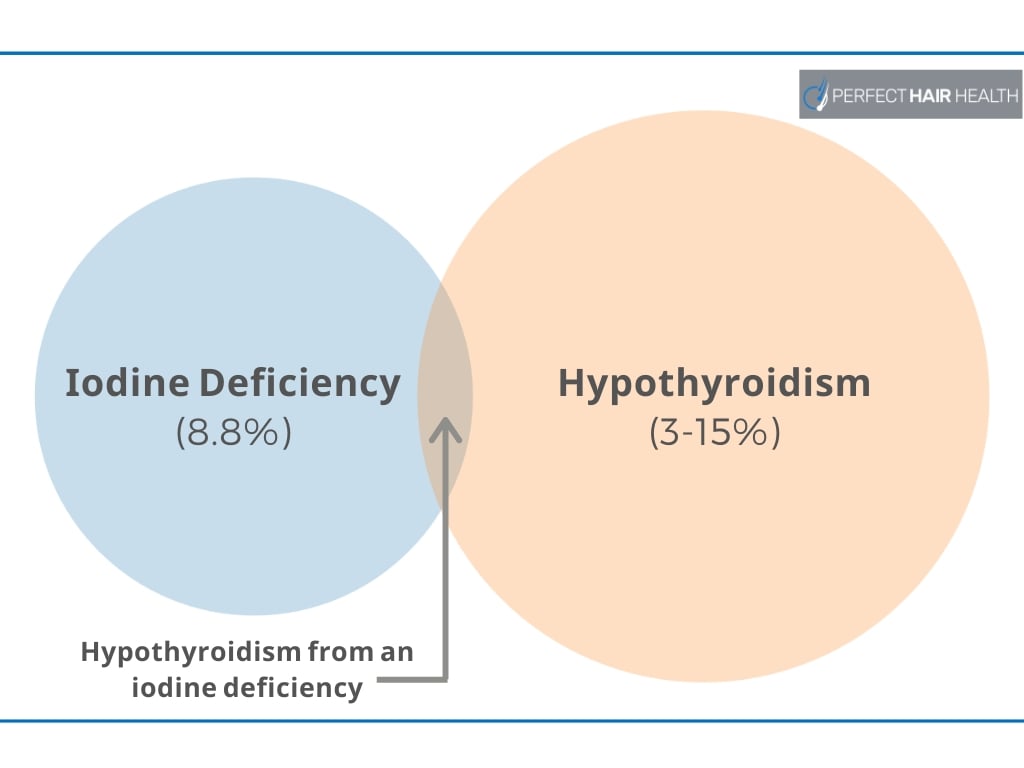
Moreover, the only scenarios where iodine deficiencies are linked to hair loss seem to occur when someone develops hypothyroidism as a result of an iodine deficiency. While subclinical hypothyroidism affects 3-15% of people in the developed world, the percent of people dealing with hypothyroidism from an iodine deficiency is only a fraction of that percent. Therefore, very few people with hair loss would benefit from an iodine supplement – if at all.
Moreover, iodine excess is associated with both hyperthyroidism and thyroid cancer. For these reasons, iodine supplementation is not only unnecessary for most hair loss sufferers, but it’s also potentially dangerous.
The bottom line? Aim to get most of your iodine from food, and avoid supplements that contain iodine. If you’re concerned of a deficiency, consider increasing your seaweed intake, reducing your exposure to goitrogens, and filtering your drinking water to remove the fluoride. This will help to ensure your iodine levels remain in that narrow therapeutic window — the middle ground that promotes health and supports hair growth.
Want help with your hair regrowth journey?
Get personalized support, product recommendations, video calls, and more from our researchers, trichologists, and PhD's dedicated to getting you the best possible outcomes.
Learn More
Perfect Hair Health Team
"... Can’t thank @Rob (PHH) and @sanderson17 enough for allowing me to understand a bit what was going on with me and why all these [things were] happening ... "
— RDB, 35, New York, U.S.A."... There is a lot improvement that I am seeing and my scalp feel alive nowadays... Thanks everyone. "
— Aayush, 20’s, Boston, MA"... I can say that my hair volume/thickness is about 30% more than it was when I first started."
— Douglas, 50’s, Montréal, CanadaWant help with your hair regrowth journey?
Get personalized support, product recommendations, video calls, and more from our researchers, trichologists, and PhD's dedicated to getting you the best possible outcomes.
Join Now - Mission Statement
 Scroll Down
Scroll Down